Meld dich an, um mehr Funktionen freizuschalten
- Speichere dieses Deck in deinem Konto
- Karteikarten mit Spaced Repetition lernen
- Als Anki (.apkg) oder PDF exportieren
- Verarbeite Dokumente mit bis zu 100 Seiten
- Bilder aus PDFs und Dokumenten extrahiert
- Bessere Textextraktion aus deinen PDFs und Dokumenten
- Bessere Karteikarten dank unseres leistungsstärkeren KI‑Modells
Karteikarten in diesem Deck (813)
-
Clinical decision: 90-year-old woman with open tibial fracture refuses surgical stabilization but accepts irrigation/debridement and antibiotics. What is the next step?
- Assess decision-making capacity
internal surgery psychiatry step2. -
Definition: What are the four criteria for medical decisional capacity?
- Consistent choice
- Understanding risks/benefits
- Understanding personal significance
- Reasoning through options
psychiatry internal step2. -
Principle: Is decisional capacity global or decision-specific?
- Decision-specific; capacity must be assessed for each decision
psychiatry internal step2. -
Legal distinction: Who determines a patient's global competence?
- Courts determine competence; physicians assess decision-specific capacity
psychiatry internal step2. -
When is discussing the case with a durable power of attorney (son) appropriate?
- If patient lacks decision-making capacity, then defer decision to durable POA
internal surgery step2. -
When is petitioning the court to appoint a guardian appropriate for a patient with incapacity?
- Only if permanently incapacitated AND no surrogate decision maker (eg, no durable POA or next of kin)
internal psychiatry step2. -
When is proceeding with recommended surgical treatment despite patient refusal justified?
- Not justified here; proceeding would violate autonomy. First assess capacity; if lacks capacity, involve durable POA rather than proceed
surgery internal ethics step2. -
When is using cast immobilization to honor a refusal appropriate for this open tibial fracture?
- Premature; if patient has capacity, abide by her refusal; if lacks capacity, decision goes to durable POA
surgery internal step2. -
Practical: How should a clinician assess the 90-year-old patient's decisional capacity for refusing surgery?
- Discuss fracture care preferences and evaluate the four capacity criteria
Answer includes image:
 internal surgery psychiatry step2.
internal surgery psychiatry step2. -
Decisional capacity assessment: who must assess it?
- Physician must assess patient's decisional capacity
internal step2. -
psychiatry step2.
-
Decisional capacity and demographics: when should assessment be done relative to age or cognitive status?
- Regardless of patient age or cognitive ability, assess capacity
neurology step2. -
Decisional capacity: concise rule combining actor, timing, and scope
- Physician assesses decisional capacity for each specific care decision, regardless of patient age or cognitive ability
 internal psychiatry step2.
internal psychiatry step2. -
Anchor: Initial step for asymptomatic elevated blood pressure (140/100) in 21-year-old
Repeat blood pressure measurements: confirm with in-office and/or at-home serial readings over weeks to months before diagnosing hypertension.
internalmedicine step2. -
Anchor: Why no additional diagnostic studies now for isolated elevated BP in asymptomatic patient
One isolated elevated reading does not diagnose hypertension; confirmation with repeat measurements required before further testing.
internalmedicine step2. -
Anchor: Primary determinants of blood pressure (3 systems)
- Renin-angiotensin-aldosterone system
- Sympathetic nervous system
- Plasma blood volume
internalmedicine step2. -
Anchor: Risk factors contributing to primary (essential) hypertension
- Advancing age
- Obesity / sedentary lifestyle
- Smoking, high-sodium diet, excess alcohol, insufficient sleep, genetics
internalmedicine step2. -
Anchor: When to measure serum aldosterone:renin ratio (hyperaldosteronism workup)
Use when secondary hypertension suspected with hypokalemia or metabolic alkalosis suggesting excess aldosterone.
internalmedicine step2. -
Anchor: Why aldosterone:renin ratio is unlikely in this patient
Patient has normal serum electrolytes (no hypokalemia) making hyperaldosteronism unlikely.
internalmedicine step2. -
Anchor: When to evaluate renal artery stenosis (renal Doppler/arteriography)
Suspect when resistant hypertension requiring multiple agents or abdominal bruit; more common from atherosclerosis (older) or fibromuscular dysplasia (younger).
internalmedicine step2. -
Anchor: Why renal artery imaging is inappropriate now for this patient
No resistant hypertension, no abdominal bruit, and patient is young without features pointing to renal artery stenosis.
internalmedicine step2. -
Anchor: Role of renal CT scan in hypertension evaluation
Not routine; may show atrophic kidneys with renal artery stenosis or used for pyelonephritis/abscess when fever, flank pain, dysuria present.
internalmedicine step2. -
Anchor: Next steps if hypertension is confirmed
Evaluate for end-organ damage and discuss lifestyle modification and antihypertensive therapy with primary care.
internalmedicine step2. -
Anchor: Educational point: long-term risks of untreated hypertension
- Heart failure
- Ischemic/hemorrhagic stroke
- Chronic kidney disease
internalmedicine step2. -
Anchor: Image: slide with highlighted text (supplemental)
Supplementary image:
 Use image only as illustration of exam explanation.internalmedicine step2.
Use image only as illustration of exam explanation.internalmedicine step2. -
internal_medicine step2.
-
internal_medicine step2.
-
Primary hypertension: major long-term complications if untreated?
- Heart failure
- Ischemic and hemorrhagic stroke
- Chronic kidney disease
internal_medicine step2. -
Primary hypertension: does a single elevated BP reading establish diagnosis?
- No. One isolated elevated BP in an asymptomatic patient does not indicate hypertension
internal_medicine step2. -
Primary hypertension: acceptable methods to confirm elevated BP before diagnosis?
- Both in-office and at-home measurements
- Or serial in-office measurements over weeks–months
 internal_medicine step2.
internal_medicine step2. -
Primary hypertension: recommended timing for serial in-office BP measurements to confirm diagnosis?
- Over a period of weeks to months
internal_medicine step2. -
Clinical decision: 18-year-old post-blunt chest trauma with left pleural effusion, tachycardia, tachypnea, rising O2 needs — most appropriate immediate management?
- Tube thoracostomy
surgery step2. -
Pathophysiology: What causes traumatic hemothorax?
- Blood in pleural space from pulmonary, bronchial, or intercostal vessel injury (eg, rib fractures)
internal_medicine step2. -
Presentation: Key clinical features of hemothorax?
- Chest pain, shortness of breath, dullness to percussion, decreased breath sounds on affected side
emergency step2. -
Definition: When is hemothorax classified as massive?
- Initial chest-tube output >1000–1500 mL or >200 mL/hr for ≥4 hr
surgery step2. -
Management decision: Purpose of initial tube thoracostomy in traumatic hemothorax?
- Promote lung expansion; exclude ongoing hemorrhage; prevent residual pneumothorax, empyema, fibrothorax, fistula
surgery step2. -
When is video-assisted thoracoscopy (VATS) or thoracotomy indicated in hemothorax?
- If massive hemothorax (see criteria) or ongoing high-volume drainage after chest tube
surgery step2. -
Ultrasonography role in blunt chest trauma with effusion: when is it appropriate?
- Useful for initial detection of pleural fluid and to guide thoracentesis, but unnecessary if CXR already shows effusion and urgent tube needed
pediatrics step2. -
CT chest role in traumatic hemothorax: when is CT appropriate?
- Characterizes injuries further (eg, vascular, parenchymal) but defer if patient needs immediate chest-tube intervention
radiology step2. -
Thoracentesis in traumatic pleural effusion: when is thoracentesis appropriate?
- Diagnostic/therapeutic for small, stable effusions or ultrasound-guided sampling; not for initial management of suspected traumatic hemothorax with respiratory compromise
internal_medicine step2. -
Comparison: Tube thoracostomy vs thoracentesis in traumatic hemothorax — main distinguishing indication?
- Tube thoracostomy: active/large hemothorax or respiratory compromise
- Thoracentesis: small, stable effusion for diagnosis/relief
surgery step2. -
Indicators of massive hemothorax (visual aid in answer)
- Massive hemothorax criteria:
- Initial chest-tube output >1000–1500 mL
- Drainage >200 mL/hr for ≥4 hr
 surgery step2.
surgery step2. -
surgery emergency step2.
-
What are chest x-ray and CT features of hemothorax?
- CXR: fluid along diaphragm with blunted costophrenic angle
- CT: hyperdense material between visceral and parietal pleura
surgery emergency step2. -
Which clinical signs mandate immediate tube thoracostomy for hemothorax?
- Tachycardia, tachypnea, increasing O2 requirements
surgery emergency step2. -
Why is tube thoracostomy preferred over thoracentesis for large/rapid hemothorax?
- Removes large blood volume + can be left in place to trend/monitor ongoing bleeding
surgery emergency step2. -
When would thoracentesis be appropriate for pleural blood?
- Diagnostic use for small/stable pleural effusion; not therapeutic for rapidly accumulating hemothorax
surgery emergency step2. -
What is the primary therapeutic goal of tube thoracostomy in hemothorax?
- Evacuate blood, prevent retained hemothorax, allow monitoring of bleeding
surgery emergency step2. -
Name complications of hemothorax (grouped into ≤3 items).
- Infectious: empyema, superimposed infection
- Pulmonary: atelectasis, fibrothorax
- Hemorrhagic: hemorrhagic shock
surgery emergency step2. -
Imaging features of hemothorax (illustration)
- CXR: blunted costophrenic angle; CT: hyperdense pleural material
 surgery emergency step2.
surgery emergency step2. -
Preoperative splenectomy: which vaccines are recommended?
- Streptococcus pneumoniae
- Haemophilus influenzae type b
- Neisseria meningitidis
 surgery internal_medicine infectious step2.
surgery internal_medicine infectious step2. -
Splenectomy: primary splenic immune functions?
- Mechanical filtration of opsonized pathogens in sinusoids
- Phagocytosis by splenic macrophages
- Houses immunoglobulin-producing B lymphocytes
internal_medicine surgery step2. -
Asplenia: which organisms cause increased severe infection risk?
- Encapsulated bacteria:
- Streptococcus pneumoniae
- Haemophilus influenzae
- Neisseria meningitidis
infectious internal_medicine step2. -
Splenectomy patients: is antibiotic prophylaxis indicated and which agents?
- May require antibiotic prophylaxis
- Typical agents: penicillin or amoxicillin
internal_medicine surgery step2. -
Why is vaccinating for S. pneumoniae, H. influenzae, and N. meningitidis before splenectomy correct?
- Spleen clears encapsulated organisms; vaccinate against the major encapsulated pathogens to reduce post-splenectomy sepsis risk
infectious surgery step2. -
Why is answer choice A (only N. meningitidis) incorrect for preoperative splenectomy vaccination?
- Choice A vaccinates only N. meningitidis; incomplete because S. pneumoniae and H. influenzae also require vaccination
internal_medicine infectious step2. -
Why is answer choice B (only H. influenzae) incorrect for preoperative splenectomy vaccination?
- Choice B vaccinates only H. influenzae; incomplete because S. pneumoniae and N. meningitidis also require vaccination
internal_medicine infectious step2. -
Why is answer choice C (H. influenzae + N. meningitidis) incorrect for preoperative splenectomy vaccination?
- Choice C omits S. pneumoniae; vaccination must include S. pneumoniae, H. influenzae, and N. meningitidis
internal_medicine infectious step2. -
Why is answer choice D (only S. pneumoniae) incorrect for preoperative splenectomy vaccination?
- Choice D vaccinates only S. pneumoniae; incomplete because H. influenzae and N. meningitidis also require vaccination
internal_medicine infectious step2. -
Why is answer choice E (S. pneumoniae + N. meningitidis) incorrect for preoperative splenectomy vaccination?
- Choice E omits H. influenzae; vaccination must include all three encapsulated organisms
internal_medicine infectious step2. -
Why is answer choice F (S. pneumoniae + H. influenzae) incorrect for preoperative splenectomy vaccination?
- Choice F omits N. meningitidis; vaccination must include S. pneumoniae, H. influenzae, and N. meningitidis
internal_medicine infectious step2. -
Acute pancreatitis: classic presentation and key symptoms
- Severe epigastric abdominal pain that radiates to the back
- Nausea and vomiting
internalmedicine pediatrics step2. -
Acute pancreatitis: common etiologies
- Gallstones
- Alcohol use
- Trauma
- Hypertriglyceridemia
- Hypercalcemia
internalmedicine surgery step2. -
Traumatic epigastric blow: diagnostic relevance
Direct blunt trauma to the epigastrium can cause acute pancreatitis
surgery pediatrics step2. -
surgery internalmedicine step2.
-
internalmedicine step2.
-
Acute pancreatitis: initial supportive management
- IV fluids (normal saline or lactated Ringer)
- Bowel rest
- Pain control
internalmedicine surgery step2. -
When is surgical intervention indicated in acute pancreatitis?
Surgery if complications develop (eg, necrosis with infection, hemorrhage, persistent pseudocyst requiring intervention)
surgery internalmedicine step2. -
Esophageal rupture: presentation and causes
- Severe retrosternal pain
- Signs of sepsis (fever, tachycardia, hypotension)
- Causes: trauma, endoscopic instrumentation, violent retching
surgery internalmedicine step2. -
Gastric ulcer: symptoms and complications
- Pain worsens with food
- Complications: perforation, stricture, upper GI bleeding (melena or hematochezia)
- Endoscopy: mucosal discontinuity/erythema
internalmedicine gastroenterology step2. -
Gastroenteritis: typical features and etiology
- Nausea, vomiting, diarrhea
- Mild generalized abdominal discomfort
- Typically infectious (viral or bacterial); not trauma-related
internalmedicine pediatrics step2. -
Hepatitis: causes and distinguishing features
- Causes: viral, autoimmune, alcohol, medications
- Features: hyperbilirubinemia with jaundice; typically chronic and not caused by blunt trauma
internalmedicine step2. -
Distinguish acute pancreatitis vs gastroenteritis (key differentiators)
- Pancreatitis: severe focal epigastric pain, nausea/vomiting, often elevated amylase/lipase
- Gastroenteritis: mild generalized pain with diarrhea, infectious, not trauma-related
internalmedicine pediatrics step2. -
Why pancreatitis is the correct diagnosis in a teen with epigastric pain after a kick
Focal severe epigastric pain after epigastric trauma with nausea/vomiting matches acute pancreatitis; trauma is a recognized cause
pediatrics surgery step2. -
What is 'postpartum endometritis' (anchor: diagnosis)?
Acute infection of the uterine endometrium after delivery, typically polymicrobial involving aerobes and anaerobes from the genital tract.
obgyn internal step2. -
Pathophysiology of postpartum endometritis (anchor: pathophysiology)?
Genital-tract microbes enter the uterine cavity during labor/delivery causing polymicrobial infection of the endometrium.
obgyn internal step2. -
Key clinical features of postpartum endometritis (anchor: clinical features)?
- Fever
- Uterine fundus tenderness
- Mucopurulent or foul-smelling lochia
- Leukocytosis
obgyn internal step2. -
Risk factors for postpartum endometritis (anchor: risk factors)?
- Cesarean delivery
- Prolonged rupture of membranes or prolonged labor
- Bacterial vaginosis
- Group B Streptococcus colonization
- Manual removal of placenta
obgyn internal step2. -
Immediate management of suspected postpartum endometritis (anchor: management)?
Start broad-spectrum IV antibiotics promptly; recommended regimen example: clindamycin plus gentamicin.
obgyn internal step2. -
Why is antibiotic therapy correct as the next step in this postpartum patient (anchor: answer-choice logic)?
Clinical picture (fever, uterine tenderness, foul lochia, leukocytosis) indicates endometritis requiring immediate broad-spectrum antibiotics.
obgyn internal step2. -
Why is CT abdomen/pelvis not the best next step for suspected endometritis (anchor: answer-choice logic)?
CT can identify intra-abdominal sources but does not confirm endometritis; it is not routinely used to diagnose endometritis.
obgyn internal step2. -
When is CT abdomen/pelvis useful after postpartum fever (anchor: diagnostics)?
To identify intra-abdominal causes such as surgical-site abscess, retained products of conception, appendicitis, or colitis.
obgyn surgery step2. -
Why is culture of the lochia not the most appropriate next step (anchor: answer-choice logic)?
Culture is not the immediate management step; treating suspected infection with antibiotics is prioritized.
obgyn internal step2. -
Why are endometrial biopsy and transvaginal ultrasound not the immediate next steps (anchor: answer-choice logic)?
They are not first-line tests to manage suspected postpartum endometritis; immediate empiric antibiotics take priority.
obgyn internal step2. -
Example presentation anchor: 36 hours postpartum with fever and foul-smelling lochia—most likely diagnosis?
Postpartum endometritis given timing, uterine tenderness, foul lochia, fever, and leukocytosis after cesarean delivery.
obgyn internal step2. -
Supplementary: slide illustrating key points about postpartum infection (anchor: visual aid)?
See slide for summarized features and management:
 obgyn internal step2.
obgyn internal step2. -
Smoking cessation and pulmonary function in a 37-year-old long-term smoker
- Smoking cessation slows the accelerated age-related decline in pulmonary function and prevents further accelerated worsening
internalmedicine pulmonary step2. -
Pathophysiology of normal aging lungs
- Loss of parenchymal scaffolding → dilation of air spaces (senile emphysema)
- ↑ alveolar dead space
internalmedicine pulmonary step2. -
Effect of smoking on age-related pulmonary decline
- Smoking increases the rate of age-related decline in pulmonary function
internalmedicine pulmonary step2. -
internalmedicine pulmonary step2.
-
Medical management for obstructive lung disease in long-term smokers
- Inhaled antimuscarinics
- Short and long-acting β-agonists
- Inhaled corticosteroids
internalmedicine pulmonary step2. -
Oxygen therapy criteria in chronic lung disease
- Resting or ambulatory O2 saturation < 88% → candidate for oxygen therapy
internalmedicine pulmonary step2. -
Lung cancer risk after smoking cessation (relation to choices B and D)
- Former smokers retain an increased lung cancer risk vs never-smokers, but risk decreases compared with continued smoking
internalmedicine oncology step2. -
Why 'pulmonary function will not decrease further' is incorrect (choice C)
- Age-related pulmonary decline normally continues from ~age 25; cessation slows but does not stop decline
internalmedicine pulmonary step2. -
Smoking and risk of myocardial infarction versus cerebral infarction (relation to choice E)
- Smoking increases risk of both myocardial and cerebral infarction via atherosclerotic buildup in coronary and intracranial arteries
internalmedicine neurology step2. -
Illustration: highlighted teaching points about smoking and lung aging
- Key points: senile emphysema, ↑ dead space, smoking accelerates decline, cessation prevents worsening
 internalmedicine pulmonary step2.
internalmedicine pulmonary step2. -
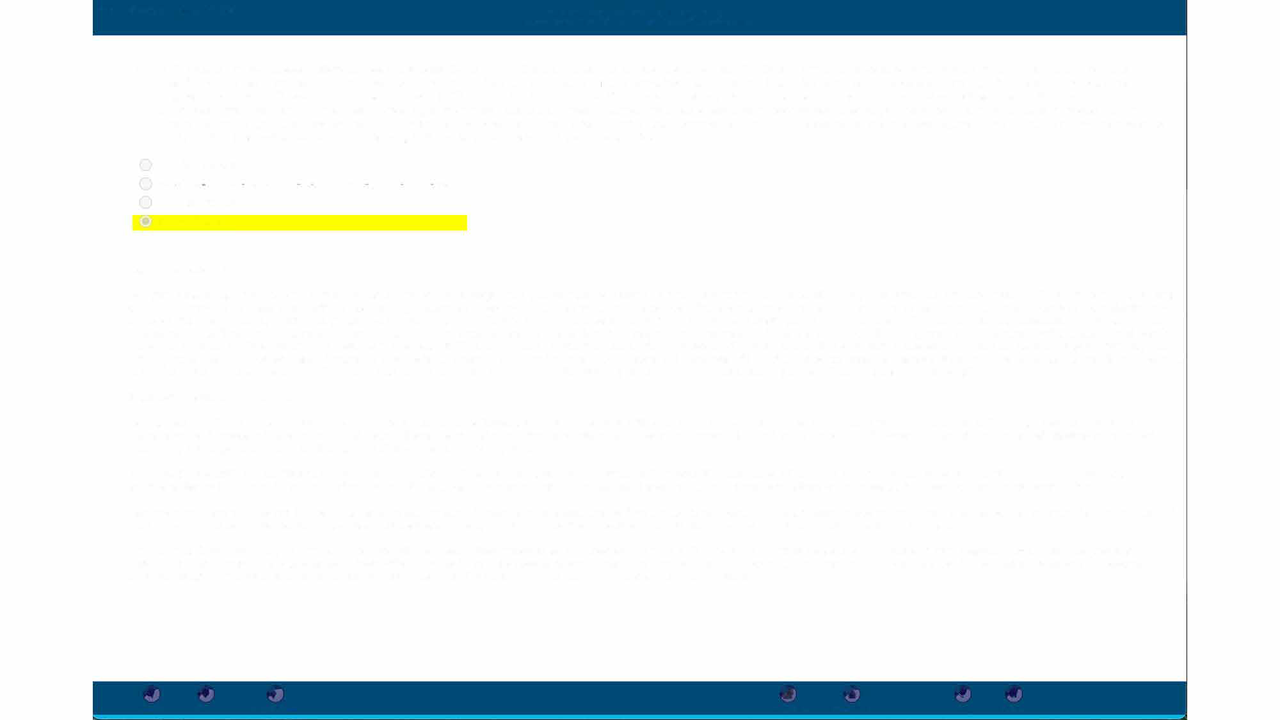
What is the diagnosis: multiple small (3–5 mm), bright red, slightly raised dome-shaped papules on trunk in a 38-year-old?
Cherry angiomas - Common benign vascular lesions - Appear after age 30
dermatology internalmedicine step2. -
dermatology internalmedicine step2.
-
What is the histologic appearance of a cherry angioma?
Congested, dilated capillaries and venules within the superficial dermis
pathology internalmedicine step2. -
What diagnostic study is most appropriate to confirm cherry angiomas?
None — no diagnostic studies required; diagnosis is clinical
dermatology internalmedicine step2. -
When is excisional biopsy appropriate for cherry angiomas?
Not required for diagnosis; biopsy/excision only if cosmetic concern or irritation
surgery dermatology step2. -
How should physicians manage patients who develop cherry angiomas?
Provide reassurance; offer removal only if desired for cosmetics/irritation
internalmedicine dermatology step2. -
Gastroenteritis: typical features and relation to blunt abdominal trauma?
Nausea, vomiting, diarrhea, mild generalized abdominal discomfort; usually infectious (viral/bacterial); not associated with abdominal trauma
infectiousdisease internalmedicine step2. -
When is acute pancreatitis likely and what lab findings support it?
Severe epigastric pain radiating to back with nausea/vomiting; can follow direct epigastric trauma; labs show ↑ serum amylase and lipase
gastroenterology internalmedicine step2. -
Hepatitis: common causes and typical presentation features?
Caused by viral infection, autoimmune disease, alcohol, or medications; often with hyperbilirubinemia/jaundice; typically chronic, not usually from blunt trauma
hepatology internalmedicine step2. -
Visual: example appearance of cherry angiomas (illustration)
Small red dome-shaped papules on trunk consistent with cherry angiomas
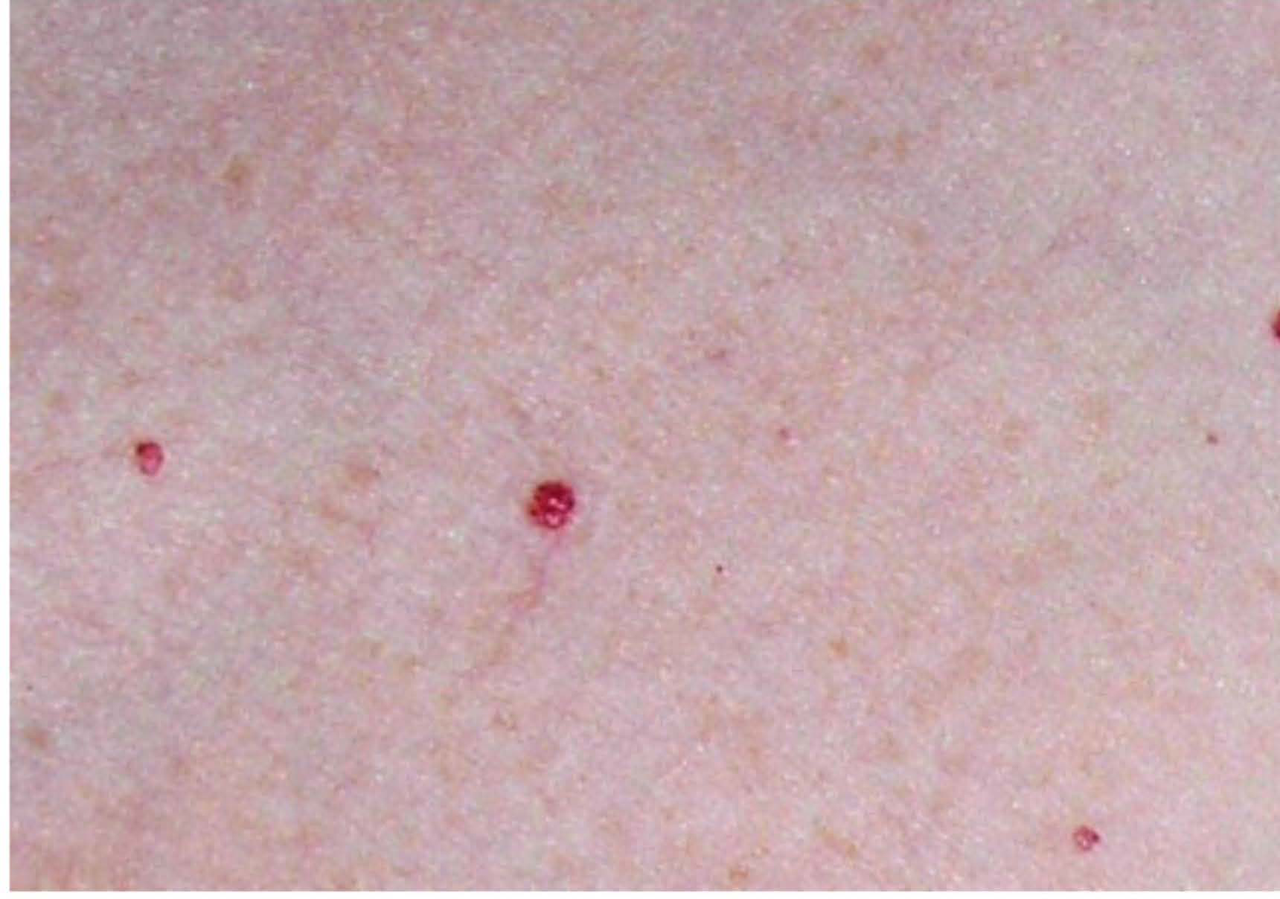 dermatology internalmedicine step2.
dermatology internalmedicine step2. -
Diagnosis: Chronic bacterial prostatitis — key presenting features in this case?
- Painful ejaculation, sometimes dark/foul ejaculate
- Chronic pelvic or low back pain (weeks–months)
- **Mildly tender, minimally enlarged prostate on DRE
internalmedicine step2 -
Risk factors: What sexual history findings increase suspicion for chronic bacterial prostatitis?
- Multiple sexual partners
- Inconsistent condom use / unprotected anal sex
- Concomitant STIs
internalmedicine step2 -
Diagnostic test: What is the two-glass test for prostatitis?
- Urine sample before prostatic massage then urine sample after prostatic massage used for microscopy/culture
internalmedicine step2 -
Diagnostic criterion: How is prostate localization established using post-massage cultures?
A ≥10-fold increase in bacterial concentration after prostatic massage localizes infection to the prostate
internalmedicine step2 -
Treatment: First-line therapy for chronic bacterial prostatitis?
- Fluoroquinolone antibiotics (prolonged courses; recurrences common)
internalmedicine step2 -
Prognosis modifiers: Factors affecting cure rates for chronic bacterial prostatitis?
- Higher cure in antibiotic-naive patients
- Lower cure with prostatic calculi
internalmedicine step2 -
Choice rationale: When is CT pelvis useful instead of two-glass test for prostate-related disease?
- CT pelvis: evaluate prostate cancer metastasis or prostatic abscess (abscess usually has systemic symptoms: fever, chills, malaise)
internalmedicine step2 -
Choice rationale: When is abdominal ultrasonography appropriate vs prostatitis testing?
- Abdominal US: evaluate pyelonephritis or kidney stones (flank pain, fever, nausea) — not for uncomplicated prostatitis
internalmedicine step2 -
Choice rationale: When is placement of urinary catheter for culture appropriate?
- Urinary catheter cultures: when patient cannot void or to evaluate suspected bacterial cystitis from obstruction; not for localizing prostate infection
internalmedicine step2 -
Diagnostic aid: Example of two-glass test visual aid
Illustration of pre- and post-prostatic massage urine collection for microscopy and culture
 internalmedicine step2
internalmedicine step2 -
Chronic bacterial prostatitis: core presenting symptoms?
- Recurrent UTI symptoms
- Pelvic/lower abdominal pain
- Dysuria or painful ejaculation
internal step2. -
Chronic bacterial prostatitis: additional possible features?
- Obstructive urinary symptoms
- Sexual dysfunction
urology step2. -
Risk factors for chronic bacterial prostatitis?
- Multiple sexual partners
- Unprotected anal sex
- Concomitant STIs
obgyn step2. -
Diagnostic test that establishes chronic bacterial prostatitis?
- Urine cultures before and after prostatic massage showing a ten-fold increase in bacterial concentration
internal step2. -
pharmacology step2.
-
infectious step2.
-
When is transrectal prostate ultrasonography useful?
- To identify prostatic calculi or prostatic abscesses
surgery step2. -
Why transrectal prostate ultrasonography is not diagnostic for chronic bacterial prostatitis?
- Findings nonspecific and insufficient to establish diagnosis; lacks sensitivity without abscess/calculi
radiology step2. -
When would transrectal ultrasonography be the correct test in prostatitis-like illness?
- Suspected prostatic abscess or suspected prostatic calculi with systemic/abscess signs
internal step2. -
Foul-smelling or dark ejaculate: suggests which diagnosis over cystitis?
- Suggests prostatic or seminal tract involvement; not consistent with isolated cystitis
infectious step2. -
Diagnosis: Key features supporting cardiogenic shock in a 76-year-old man
- Hypotension (BP 84/56 → 78/42)
- Pulmonary edema (diffuse crackles, respiratory distress, low O2 sat)
- Elevated JVD to angle of jaw
- Low EF (10%) after anterior MI
internal_medicine cardiology step2. -
Pathophysiology: How cardiogenic shock causes hypotension and pulmonary edema
- Pump failure → reduced cardiac output → hypotension
- ↑Left-sided end‑diastolic pressure → pulmonary venous congestion → pulmonary edema
internal_medicine cardiology step2. -
Management: First-line pharmacologic therapy for cardiogenic shock after MI
- Dobutamine (inotropic support) often first-line; may combine with vasopressor if needed
internal_medicine cardiology step2. -
Drug: Dobutamine mechanism relevant to cardiogenic shock
- β1 agonist → ↑contractility, ↑HR, ↑cardiac output
- Modest α1 activity → modest ↑peripheral vascular tone to help MAP
internal_medicine cardiology step2. -
Drug: Norepinephrine role in cardiogenic shock
- α‑agonist predominance → strong vasoconstriction to raise MAP
- Minimal inotropy; used alone or with dobutamine if vasoplegia or severe hypotension
internal_medicine cardiology step2. -
Comparison: Dobutamine vs Norepinephrine in cardiogenic shock
- Dobutamine: primary inotrope (↑CO)
- Norepinephrine: primary vasopressor (↑MAP)
- Use dobutamine for pump failure; add norepinephrine if MAP remains low
internal_medicine cardiology step2. -
Drug: Why vasopressin (ADH) is not first-line for cardiogenic shock
- V1 receptor → vasoconstriction ↑MAP
- No inotropy; causes reflex ↓HR and ↓cardiac output → worsens pump failure
internal_medicine pharmacology step2. -
Drug: Why isoproterenol is harmful after acute MI with cardiogenic shock
- Nonselective β agonist → ↑HR and contractility but ↓SVR → ↓coronary perfusion and ↑myocardial O2 demand → worsens ischemia
internal_medicine cardiology step2. -
Drug: Why phenylephrine is not recommended as first-line in cardiogenic shock
- Pure α1 agonist → ↑afterload and peripheral resistance
- No inotropy; ↑afterload may reduce stroke volume and cardiac output in pump failure
internal_medicine pharmacology step2. -
Clinical decision: When to add a vasopressor to dobutamine in cardiogenic shock
- Add vasopressor (eg, norepinephrine) if mean arterial pressure remains low despite inotropic support
internal_medicine cardiology step2. -
Visual aid: Dobutamine mechanism and effect on hemodynamics (image on answer)
- Dobutamine: β1 → ↑contractility and CO; modest α1 → mild ↑SVR
 internal_medicine cardiology step2.
internal_medicine cardiology step2. -
Cardiogenic shock: defining clinical presentation?
- Hypotension
- Evidence of end-organ damage
- Context: acute decompensated heart failure
internalmedicine cardiology step2. -
Cardiogenic shock: first-line therapy?
- Inotropic support (first-line)
- Examples: dobutamine or dopamine
internalmedicine cardiology step2. -
Dobutamine: role in cardiogenic shock?
- Inotropic agent recommended as a first-line option for cardiogenic shock
internalmedicine cardiology step2. -
Dopamine: role in cardiogenic shock?
- Inotropic agent recommended as a first-line option for cardiogenic shock
internalmedicine cardiology step2. -
Norepinephrine: role in cardiogenic shock?
- Vasopressor adjunct: may be used in conjunction with inotropic agents
internalmedicine cardiology step2. -
Cardiogenic shock: summary slide (visual aid)?
Slide shows key points: hypotension, end-organ damage, first-line inotropes (dobutamine, dopamine), norepinephrine adjunct.
 internalmedicine cardiology step2.
internalmedicine cardiology step2. -
Upper-extremity deep venous thrombosis (UEDVT): key pathophysiology
- Thoracic outlet compression injures axillary/subclavian vein with repetitive use
- Repetitive vigorous upper-extremity activity predisposes to thrombosis
internalmedicine step2. -
Upper-extremity DVT: typical clinical presentation
- Young healthy athlete after vigorous upper-body exercise
- Arm/shoulder/neck pain, unilateral swelling, bluish forearm/hand discoloration
- Dilated superficial collateral veins (Urschel sign)
internalmedicine step2. -
Why is venous thrombosis the most likely cause of this patient's unilateral arm swelling?
- Presentation matches UEDVT: recent vigorous upper-body activity, unilateral edema, bluish discoloration, prominent superficial chest/shoulder veins
internalmedicine step2. -
Diagnosis of upper-extremity DVT: preferred test and finding
- Doppler ultrasonography showing a noncompressible vessel with intravascular thrombus
 internalmedicine step2.
internalmedicine step2. -
internalmedicine step2.
-
Arterial occlusion: when would this explain limb findings?
- Acute limb ischemia with severe pain, pallor, paresthesia, pulselessness, poikilothermia (not isolated swelling)
surgery step2. -
Compartment syndrome: pathophysiologic mechanism
- Compartment pressure ≈/> diastolic BP → impaired blood flow → ischemia of compartment and downstream structures
surgery step2. -
Hematoma: clinical clues making it the correct cause of limb swelling
- Focal, palpable collection after trauma or in anticoagulated patients; large hematoma would be evident on exam
surgery step2. -
Lymphedema: distinguishing features vs venous obstruction
- Causes: lymphatic obstruction/excision (eg, node dissection, lymphoma)
- Usually localized to a limb; no dilated superficial veins because venous drainage intact
internalmedicine step2. -
UEDVT epidemiology and typical setting
- UEDVT is rare; often occurs in young healthy patients after vigorous upper-extremity activity and thoracic outlet anatomy abnormalities
internalmedicine step2. -
Bacterial tracheitis: key presenting signs in a child
- Severe cough
- Inspiratory stridor
- High fever
- Intercostal/suprasternal retractions
- Generally clear lung sounds
pediatrics infectious step2. -
Bacterial tracheitis: typical causative organisms
- Streptococcus pneumoniae
- Haemophilus influenzae
- Staphylococcus aureus
pediatrics infectious step2. -
Bacterial tracheitis: characteristic chest x-ray finding
- Tracheal air column with irregular ('shaggy') borders; may have peribronchial cuffing
radiology pediatrics step2. -
Bacterial tracheitis: first-line management
- IV antibiotics plus corticosteroids; admit for monitoring; intubate if respiratory failure
pediatrics internal_medicine step2. -
Why is croup (laryngotracheobronchitis) less likely in this child?
- No improvement after 2 doses of nebulized racemic epinephrine, making bacterial tracheitis more likely
pediatrics infectious step2. -
When is epiglottitis the correct diagnosis instead of bacterial tracheitis?
- Acute severe throat pain, drooling, difficulty swallowing, muffled voice, trismus, visible swollen epiglottis
pediatrics emergency step2. -
When is bronchiolitis the correct diagnosis instead of bacterial tracheitis?
- Infant/young child with runny nose, cough, tachypnea, wheezing, often due to RSV; usually low-grade fever
pediatrics infectious step2. -
When is peritonsillar abscess the correct diagnosis instead of bacterial tracheitis?
- Sore throat, unilateral tonsillar swelling, trismus, drooling, fever, difficulty opening mouth
otolaryngology pediatrics step2. -
Bacterial tracheitis: diagnosis cues and role of imaging
- Diagnosis clinical: severe cough, high fever, stridor, clear lungs; chest x-ray may show 'shaggy' tracheal air column (see image)
 pediatrics radiology step2.
pediatrics radiology step2. -
Bacterial tracheitis: what is the definition?
Potentially serious bacterial upper respiratory infection of the trachea.
pediatrics step2. -
Bacterial tracheitis: common presenting respiratory signs/symptoms?
- Cough
- Increased work of breathing
- Stridor
pediatrics step2. -
internal_medicine step2.
-
internal_medicine step2.
-
Bacterial tracheitis: chest x-ray finding?
Tracheal air column with irregular borders on chest x-ray.
radiology step2. -
Bacterial tracheitis: first-line management components?
- Antibiotics
- Corticosteroids
- Often hospitalization
pediatrics internal_medicine step2. -
surgery step2.
-
Bacterial tracheitis: supportive image illustrating tracheal air column (useful but not required to answer)
Chest x-ray may show a tracheal air column with irregular borders.
 radiology step2.
radiology step2. -
ECMO decision for a 37-year-old woman with cystic fibrosis, recurrent pulmonary failure, and refusal of lung transplant: what is the appropriate assessment?
- ECMO is unlikely to change the patient's outcome
internalmedicine surgery step2. -
Patient competence in treatment decisions: what is the documented status for this patient?
- Mentally competent per psychologic testing during the past year
psychiatry internalmedicine step2. -
Scope of the patient's living will in this case:
- No cardiopulmonary resuscitation (no CPR) if cardiac arrest while hospitalized
internalmedicine ethics step2. -
Relevance of the patient's repeated refusal of lung transplant to decision-making:
- Patient repeatedly refused consideration for lung transplant
internalmedicine ethics step2. -
Current respiratory support status of the patient in the ICU:
- Heavily sedated, intubated, and mechanically ventilated
criticalcare internalmedicine step2. -
Why does the living will not automatically prohibit ECMO in this patient?
- Living will specifies no CPR only; it does not state refusal of ECMO
internalmedicine ethics step2. -
When should family members initiate medical treatment plans for a hospitalized patient?
- When the patient lacks decision-making capacity; not when patient is documented competent
ethics internalmedicine step2. -
Gastroenteritis: typical features described in the text
- Nausea, vomiting, diarrhea, mild generalized abdominal discomfort; typically infectious and self-limiting
internalmedicine pediatrics step2. -
Acute pancreatitis: characteristic clinical presentation
- Severe epigastric pain radiating to the back with nausea and emesis
internalmedicine surgery step2. -
internalmedicine surgery step2.
-
Acute pancreatitis: possible relation to trauma per the text
- Can occur after direct abdominal trauma to the epigastric region
surgery trauma step2. -
Hepatitis: typical features and causes mentioned
- Causes: viral, autoimmune, alcohol, medications; feature: hyperbilirubinemia with jaundice; typically chronic
internalmedicine infectiousdisease step2. -
Chronic transplant nephropathy: key pathophysiologic mechanism?
- CD4+ T cell response to donor peptides (eg, MHC) → cytokines → humoral (type II) + cellular (type IV) injury → vascular arteriosclerosis, smooth muscle proliferation → parenchymal fibrosis and atrophy
internal_medicine step2. -
Chronic transplant nephropathy: typical clinical manifestations?
- Progressive transplant dysfunction over months–years → fatigue, anorexia, edema; rising BUN/creatinine and anemia as in this patient (BUN 50 mg/dL, Cr 5.3 mg/dL, Hb 8 g/dL)
internal_medicine step2. -
Chronic transplant nephropathy: diagnostic evaluation?
- Serum/urine tests, kidney ultrasonography, biopsy showing arteriosclerosis, fibrosis, atrophy
internal_medicine step2. -
Chronic transplant rejection: response to standard immunosuppression?
- Not adequately prevented by immunosuppressive therapy; leads to organ failure and may require dialysis or repeat transplant
internal_medicine step2. -
Acute cellular rejection of a renal allograft: immune mediator and timing?
- CD8+ T lymphocytes recognizing donor class I MHC on graft cells; occurs within 6–12 months posttransplant and responds to increased immunosuppression
internal_medicine step2. -
Gastroenteritis: typical features that distinguish it from transplant failure?
- Nausea, vomiting, diarrhea, mild generalized abdominal discomfort; usually viral or bacterial and self-limited, not linked to progressive renal dysfunction
internal_medicine step2. -
Examples of chronic rejection in other transplanted organs
- Liver: vanishing bile duct syndrome
- Lung: bronchiolitis obliterans
- Heart: accelerated atherosclerosis
internal_medicine step2. -
Chronic transplant nephropathy: illustrative biopsy/ultrasound as supplement
Image: chronic transplant changes (arteriosclerosis, fibrosis, atrophy) shown for illustration
 internal_medicine step2.
internal_medicine step2. -
Viral hepatitis: key lab pattern suggesting acute viral hepatitis in this case
- Markedly ↑ AST/ALT (AST 1095, ALT 1300 U/L)
- Hyperbilirubinemia (total 11 mg/dL, direct 2.2 mg/dL)
- Normal leukocyte count (5800/mm3)
internal_medicine step2. -
Viral hepatitis: common causes of acute hepatitis listed
- Viral infections
- Alcohol, medications
- Autoimmune disease, ischemic injury
internal_medicine step2. -
Viral hepatitis: common presenting symptoms
- Fatigue, nausea, vomiting
- Right upper quadrant pain, jaundice, pruritus, abdominal distension
internal_medicine step2. -
Viral hepatitis: initial serologic tests mentioned
- Anti-hepatitis A IgM and IgG
- Anti-hepatitis C IgM and IgG
- Multiple anti-HBV antibodies and antigens
infectious_disease internal_medicine step2. -
Viral hepatitis: initial management approach
- Supportive care
- Treat complications (metabolic abnormalities, hepatic encephalopathy)
- Pursue specific therapy after identifying cause
internal_medicine step2. -
Cholangitis: clinical features and typical labs that distinguish it from viral hepatitis
- Features: fever, jaundice, RUQ pain (Charcot triad)
- Labs: leukocytosis, ↑ALP, ↑GGT, ↑bilirubin; transaminase rise usually milder than hepatitis
surgery internal_medicine step2. -
Cholecystitis: presentation and typical lab expectations
- Presentation: RUQ pain, fever, leukocytosis; usually due to cystic duct obstruction (gallstone)
- Labs: bile duct usually patent → ALT/AST and bilirubin often not elevated unless concomitant cholangitis/choledocholithiasis
surgery internal_medicine step2. -
Choledochal cyst: typical age, symptoms, and usual lab findings
- Age: often <10 years but can present in adults
- Symptoms: abdominal pain, jaundice, palpable mass, nausea/vomiting
- Labs: usually normal liver enzymes (biliary duct often not obstructed)
pediatrics surgery step2. -
Comparison: Why viral hepatitis fits this patient vs cholangitis or cholecystitis
- Viral hepatitis fits: marked ALT/AST rise + normal leukocytes
- Cholangitis expects: leukocytosis + cholestatic pattern (↑ALP/GGT)
- Cholecystitis expects: leukocytosis and localized gallbladder disease without major transaminase rise
internal_medicine surgery step2. -
Viral hepatitis: illustrative slide of teaching points (image on answer side)
Key tests and features summarized below.

- Marked ↑ AST/ALT; hyperbilirubinemia; normal WBC
internal_medicine infectious_disease step2. -
Acute viral hepatitis: key clinical features?
- Fatigue
- Nausea/vomiting
- RUQ pain
- Jaundice
- Pruritus
- Abdominal distension
internal_medicine step2. -
internal_medicine step2.
-
Viruses often implicated in acute viral hepatitis (group 1)?
- Hepatitis A virus (HAV)
- Hepatitis B virus (HBV)
- Hepatitis C virus (HCV)
internal_medicine infectious_disease step2. -
Viruses often implicated in acute viral hepatitis (group 2)?
- Varicella zoster virus (VZV)
- Cytomegalovirus (CMV)
- Epstein-Barr virus (EBV)
- Herpes simplex virus 1/2 (HSV-1/2)
internal_medicine infectious_disease step2. -
Acute viral hepatitis: initial management approach?
Supportive care; treat complications until specific antiviral chosen after virus ID
internal_medicine step2. -
internal_medicine step2.
-
Pancreatic pseudocyst: patient population and frequency?
Occurs in about 10% of patients with chronic pancreatitis
surgery internal_medicine step2. -
Pancreatic pseudocyst: common presenting symptoms when symptomatic?
- Abdominal pain
- Early satiety
- Weight loss (from mass effect)
surgery internal_medicine step2. -
Acute pancreatitis: typical clinical presentation?
- Epigastric pain
- Nausea/vomiting
- Often with gallstones, alcohol, or trauma
surgery internal_medicine step2. -
surgery internal_medicine step2.
-
Pancreatitis: diagnostic lab marker specificity?
Elevated lipase is a specific indicator of pancreatitis
internal_medicine step2. -
Why acute viral hepatitis is more likely than pancreatitis in a patient with very large ALT/AST rise and no clear pancreatitis history?
Because acute viral hepatitis produces large acute ALT/AST increases; pancreatitis usually causes prominent abdominal pain and elevated lipase
internal_medicine step2. -
When would pancreatitis be the correct diagnosis instead of acute viral hepatitis?
When patient has epigastric pain, nausea/vomiting, risk factors (gallstones, alcohol), and elevated lipase
surgery internal_medicine step2. -
When would pancreatic pseudocyst explain symptoms instead of acute viral hepatitis?
When chronic pancreatitis history plus mass symptoms (early satiety, weight loss, abdominal pain) suggest a pseudocyst
surgery internal_medicine step2. -
Clinical diagnosis: 9-year-old with 5-month intermittent right flank pain, absent left kidney on ultrasound, severe dilation of right renal pelvis. What is the clinical problem?
- Single functioning kidney with hydronephrosis
pediatrics surgery step2. -
Pathophysiology: How does vesicoureteral reflux lead to kidney failure?
- Reflux → hydroureter/hydronephrosis → compression atrophy (reflux nephropathy) → progressive renal parenchymal loss
pediatrics internalmedicine step2. -
Key management: Most appropriate immediate intervention to prevent progression of renal failure from proximal ureteral obstruction in a single kidney?
- Insert percutaneous nephrostomy tube (temporary decompression)
surgery pediatrics step2. -
Rationale: Why is percutaneous nephrostomy preferred here?
- Directly decompresses proximal obstruction/hydronephrosis to preserve renal parenchyma before definitive repair
surgery pediatrics step2. -
When is a urinary catheter the correct immediate intervention for urinary obstruction?
- Bladder outlet obstruction (eg, urethral stricture/retention) with overflow incontinence or palpable suprapubic mass
urology pediatrics step2. -
Why is a urinary catheter NOT appropriate for this patient?
- Obstruction is proximal (ureteral), not bladder outlet; catheter won't decompress hydronephrosis
surgery pediatrics step2. -
When is cystoscopy with bladder outlet dilatation appropriate for urinary obstruction?
- Distal bladder outlet obstruction amenable to endoscopic dilation (eg, urethral stricture, posterior urethral valves)
urology pediatrics step2. -
Why is cystoscopy with bladder outlet dilatation NOT appropriate for this patient?
- No bladder outlet obstruction signs; imaging shows proximal ureteral/renal pelvis dilation
surgery pediatrics step2. -
When is intravenous furosemide indicated in renal/volume management?
- Acute hypervolemia (eg, pulmonary edema from heart failure) to increase diuresis
internalmedicine pediatrics step2. -
Why is intravenous furosemide inappropriate in obstruction-related hydronephrosis?
- Increasing urine production with outflow obstruction can worsen postrenal azotemia and hydronephrosis
internalmedicine pediatrics step2. -
When is IV 0.9% saline bolus indicated in acute management?
- Hypovolemia or distributive shock with signs of volume depletion (eg, hypotension, dry mucous membranes)
internalmedicine pediatrics step2. -
Why is IV 0.9% saline bolus inappropriate for this patient?
- No hypovolemia signs; extra intravascular volume may worsen hydronephrosis and renal injury
internalmedicine pediatrics step2. -
Congenital urinary tract anomalies associated with ureteral obstruction or reflux (examples relevant to single-kidney patients)
- Unilateral renal agenesis,
- Duplex collecting system,
- Ureteral stricture/stenosis
pediatrics surgery step2. -
Clinical priority in patients with unilateral renal agenesis
- Preserve function of the solitary kidney (prevent obstruction/reflux injury)
pediatrics internalmedicine step2. -
Ultrasound finding anchor: Absent left kidney and severe right renal pelvic dilation implies what immediate risk?
- High risk of progressive renal parenchymal loss and kidney failure from obstruction
radiology pediatrics step2. -
Supplement: Illustration of hydronephrosis in single kidney—useful for visualizing severe renal pelvis dilation
- See image for renal pelvic dilation:

- Image is illustrative only; diagnosis based on ultrasound and clinical features above
radiology pediatrics step2. - See image for renal pelvic dilation:
-
Percutaneous nephrostomy tube: primary clinical indication?
- Temporary drainage to prevent progression of kidney failure
- When definitive management of vesicoureteral reflux or ureteral obstruction is pending
surgery pediatrics internal_medicine step2. -
Vesicoureteral reflux (VUR) or ureteral obstruction: role of percutaneous nephrostomy?
- Bridge therapy: provides temporary urinary diversion before definitive repair of VUR or relief of obstruction
urology surgery step2. -
Percutaneous nephrostomy tube: intended immediate benefit to renal function?
- Prevents progression of kidney failure by decompressing obstructed urinary tract
nephrology internal_medicine step2. -
Anchor: Nonadherence in 21-year-old with type 2 diabetes; defining features?
- Age 21, type 2 diabetes, A1c 9%, admits not checking glucose to be 'like everyone else', on metformin + glipizide
internal_medicine step2 -
Anchor: Best physician approach for young diabetic nonadherent due to social perception
- Organize multidisciplinary care + peer support group for young patients with diabetes
internal_medicine psychiatry step2 -
Anchor: Why multidisciplinary care + peer support is correct for social-perception nonadherence?
- Addresses emotional/social causes, connects patient with similar peers, improves disease perception and adherence
psychiatry internal_medicine step2 -
Anchor: When is contacting a patient's parent appropriate?
- Appropriate when patient lacks decision-making capacity; otherwise contacting parent breaches trust and HIPAA
internal_medicine ethics step2 -
Anchor: When is a mobile glucose app likely effective for nonadherence?
- Effective when barrier = difficulty/complexity of monitoring; not effective when barrier = social desire to fit in
internal_medicine step2 -
Anchor: When is scare/threatening counseling (eg, 'you will be blind') appropriate?
- Scare tactics are inappropriate; education about complications should be empathetic and nonthreatening
internal_medicine psychiatry step2 -
Anchor: Use of humor with a patient admitting nonadherence due to social stigma
- Humor may damage rapport here; prefer empathetic, nonjudgmental, open-ended inquiry
psychiatry internal_medicine step2 -
Anchor: Clinical communication principle for nonadherence evaluation
- Use open-ended, curious, nonjudgmental questions to identify root cause before planning interventions
psychiatry internal_medicine step2 -
Anchor: Study-note rule: overriding refusals or contacting others
- Assess decision-making capacity before overriding refusals or notifying others
internal_medicine ethics step2 -
Anchor: Choice E — strengthen physician-patient relationship. Why is this option insufficient for treatment nonadherence?
Strengthening relationship is humanistic but does not address underlying nonadherence drivers; the patient needs multi‑front support to realize others share his experience.
internalmedicine step2. -
Anchor: Treatment nonadherence. Common practical reasons (group A)?
- Financial strains
- Treatment side effects
- Poor health literacy causing misunderstanding
internalmedicine step2. -
Anchor: Treatment nonadherence. Common psychosocial reasons (group B)?
- Social perception or judgment
- Mental/emotional strain from adjustment
psychiatry step2. -
Anchor: Approach to a nonadherent patient. What clinician attitude is recommended?
Use an open‑ended, curious, nonjudgmental approach to explore reasons for nonadherence.
internalmedicine step2. -
Anchor: When is peer support indicated for a nonadherent patient?
When the patient needs reassurance that many others share his experience and multi‑front support beyond the clinician relationship.
psychiatry step2. -
Anchor: Use of image. What supplementary purpose can a highlighted slide image serve when teaching about nonadherence?
Illustrate emphasized teaching points; image as supplement only, not as sole source of the answer.
 internalmedicine step2.
internalmedicine step2. -
Diagnosis: Tingling in left ring and small fingers + medial forearm sensory loss in a 62-year-old with left arm dialysis fistula — most likely diagnosis?
- Ulnar nerve compression
neurology internal_medicine step2. -
Pathophysiology: How does an elbow arteriovenous fistula cause neuropathy?
- AV fistula at elbow → local compression/traction of ulnar nerve
neurology surgery step2. -
Feature: Sensory distribution of ulnar nerve compression at the elbow?
- Numbness/paresthesia: ring and small fingers; medial hand; medial forearm to elbow
neurology step2. -
Feature: Motor findings expected with ulnar nerve compression at the wrist vs elbow?
- Wrist compression → hand weakness and intrinsic atrophy; Elbow compression → sensory ± weakness
neurology step2. -
Diagnostic test to confirm suspected ulnar nerve compression?
- Electrodiagnostic testing (nerve conduction/EMG)
neurology internal_medicine step2. -
Initial management for ulnar nerve compression related to dialysis fistula?
- Behavior modification and ergonomic measures
neurology surgery step2. -
When is surgery indicated for ulnar nerve compression?
- Severe or refractory symptoms after conservative measures
surgery neurology step2. -
Arteriovenous steal syndrome: when would this diagnosis fit in a dialysis patient?
- Ischemic distal limb signs: pallor, pain during dialysis, pain at rest; uncommon to localize only to ring/small fingers
internal_medicine nephrology step2. -
Why is diabetic neuropathy unlikely to explain isolated ring/small finger and medial forearm sensory loss?
- Diabetic neuropathy causes symmetric distal polyneuropathy, not focal ulnar distribution
neurology internal_medicine step2. -
Why are central causes (eg, cerebral infarction) unlikely for isolated medial hand and forearm sensory loss?
- Cerebral infarction causes contralateral cortical or hemispheric deficits, not focal peripheral nerve distribution to ring/small fingers and medial forearm
neurology internal_medicine step2. -
Use of provided image: What clinical sign near a dialysis fistula suggests local hemodynamic device presence without inflammation?
- Palpable thrill at fistula site
 internal_medicine surgery step2.
internal_medicine surgery step2. -
Essential (pre-existing) hypertension in pregnancy: diagnostic blood pressure criteria and timing?
- Systolic > 140 mm Hg or diastolic > 90 mm Hg
- On ≥2 measurements ≥4 hours apart
- Before 20 weeks' gestation
obgyn internal step2. -
Why is the 37-year-old patient in the vignette diagnosed with essential hypertension?
- BP 150/100 and 150/98 at 18 wk (before 20 wk) with trace urine protein → meets pre-existing HTN criteria; urine protein can be normal in essential HTN
obgyn internal step2. -
Normal urine protein result significance in essential hypertension during pregnancy?
- Urine protein often normal in essential (pre-existing) hypertension
obgyn internal step2. -
Gestational hypertension: when would this diagnosis apply?
- New hypertension after 20 weeks' gestation without proteinuria
obgyn internal step2. -
Preeclampsia: defining feature that distinguishes it from essential hypertension?
- Hypertension with new proteinuria or end-organ dysfunction after 20 weeks' gestation
obgyn internal step2. -
Superimposed preeclampsia on essential hypertension: when is this diagnosis correct?
- Patient has pre-existing hypertension before 20 wk and then develops new proteinuria or worsening HTN/end-organ signs
obgyn internal step2. -
Transient hypertension in pregnancy: defining features?
- Temporary BP elevation without persistent hypertension and no proteinuria, typically resolves
obgyn internal step2. -
Physiologic blood pressure change in early pregnancy relevant to diagnosis?
- BP decreases between 12 and 19 weeks' gestation, which can mask pre-existing HTN
obgyn internal step2. -
Maternal and fetal risks associated with essential hypertension in pregnancy?
- Mother: superimposed preeclampsia, postpartum hemorrhage
- Fetus: fetal growth restriction, preterm birth, placental abruption
obgyn internal step2. -
Initial management principles for essential hypertension in pregnancy?
- Oral antihypertensives and increased maternal-fetal monitoring
obgyn internal step2. -
Slide image: visual highlight of teaching points (supplementary)
- Supplementary image:
- Image illustrates highlighted teaching points; question answers must be known without the image
obgyn internal step2. - Supplementary image:
-
Diagnosis: 42-year-old transplant patient with Ca2+ 11.7 mg/dL and PTH 425 pg/mL; chronic kidney failure history. What is the most likely diagnosis?
- Tertiary hyperparathyroidism
internal_medicine surgery step2. -
Pathophysiology: What causes tertiary hyperparathyroidism in chronic kidney disease?
- Long-term secondary hyperparathyroidism → parathyroid hyperplasia → autonomous PTH secretion → persistent hypercalcemia
internal_medicine surgery step2. -
Lab pattern: What combination of serum calcium and PTH occurs in tertiary hyperparathyroidism?
- Elevated serum Ca2+ with persistently elevated PTH
internal_medicine step2. -
Treatment: Primary management for tertiary hyperparathyroidism?
- Surgical removal of one or more hyperplastic parathyroid glands
 surgery internal_medicine step2.
surgery internal_medicine step2. -
Why is hypervitaminosis D (excess vitamin D) an unlikely cause of this patient's labs?
- Hypervitaminosis D → hypercalcemia but causes suppressed PTH via negative feedback
internal_medicine step2. -
When would hypervitaminosis A be the correct diagnosis instead of tertiary hyperparathyroidism?
- Excess vitamin A with symptoms: dry/itchy skin, hair loss, headaches, nausea/vomiting, fatigue, irritability, joint pain
internal_medicine step2. -
Why is parathyroid adenoma (primary hyperparathyroidism) less likely in this patient with CKD history?
- CKD history more consistent with tertiary hyperparathyroidism from hyperplasia; text states parathyroid adenoma would present with decreased PTH concentrations
internal_medicine step2. -
Why is thyrotoxicosis an unlikely explanation for this patient's hypercalcemia and PTH elevation?
- Thyrotoxicosis causes hyperthyroid symptoms (palpitations, tremor, weight loss) and involves thyroid hormones, not autonomous PTH secretion
internal_medicine step2. -
Clinical features of hyperparathyroidism to recognize in patients:
- Fatigue; muscle weakness; bone pain; kidney stones
internal_medicine step2. -
Distinguishing parathyroid hyperplasia vs adenoma in hyperparathyroidism context:
- Hyperplasia: multiple glands enlarged, occurs in long-term secondary → tertiary; Adenoma: single gland, primary disease
internal_medicine surgery step2. -
Define the procedure parathyroidectomy.
- Parathyroidectomy: operation to remove one or more hyperplastic parathyroid glands.
 surgery step2.
surgery step2. -
Meningococcal disease: key clinical presentation
- Fever
- Headache
- Nuchal rigidity
- Altered mental status
- Often preceded by upper respiratory prodrome
internalmedicine step2. -
Neisseria meningitidis: important epidemiologic risk factor
- Communal living (eg, homeless shelters) increases risk of meningococcal disease
infectiousdisease internalmedicine step2. -
Definition of 'close contacts' for meningococcal prophylaxis
- Close contact = proximity within feet for >8 hours or direct exposure to oral secretions
infectiousdisease internalmedicine step2. -
Management anchor: appropriate prophylaxis strategy for hospital personnel exposed to N. meningitidis
- Chemoprophylaxis for close contacts only
internalmedicine step2. -
Why prophylaxis for close contacts is correct for meningococcal exposure
- Chemoprophylaxis decreases spread; close contacts (prolonged proximity or oral secretions) are highest risk
infectiousdisease internalmedicine step2. -
Why prophylaxis for all ED personnel on arrival (Choice A) is incorrect
- Not necessary: personnel not in vicinity for prolonged time are low risk; avoid unnecessary antibiotics and resistance
internalmedicine infectiousdisease step2. -
Why prophylaxis for immunocompromised personnel only (Choice C) is incorrect
- Not inclusive: immunocompetent close contacts are also at risk and should receive prophylaxis
internalmedicine infectiousdisease step2. -
Why no prophylaxis for hospital personnel (Choice D) is incorrect
- Not appropriate: chemoprophylaxis has been shown to decrease transmission among close contacts
infectiousdisease internalmedicine step2. -
pharmacology internalmedicine step2.
-
pharmacology internalmedicine step2.
-
Diagnosis: What diagnosis is most consistent with acute onset severe dyspnea, hypoxemia (SpO2 88%), sinus tachycardia, 1+ bilateral leg edema, recent long-distance immobility (truck driving), and a chest x-ray shown?
- Acute pulmonary embolism (PE)
internal_medicine step2 -
Pathophysiology: What ABG pattern is associated with acute pulmonary embolism?
- Acute respiratory alkalosis with hypoxemia and increased A–a gradient
internal_medicine step2 -
Risk factors: Which immobility-related risk is highlighted for PE in this case?
- Prolonged sitting (long-distance truck driving)
internal_medicine step2 -
Diagnostic test choice: What is the preferred imaging to confirm suspected acute pulmonary embolism?
- Spiral CT scan of the chest (CT pulmonary angiography)
internal_medicine step2 -
D-dimer use: When is a serum D-dimer assay appropriate for suspected PE?
- When clinical suspicion is low but PE cannot be excluded
internal_medicine step2 -
BNP use: When is serum BNP measurement indicated instead of primary PE testing?
- When concern is for congestive heart failure/cardiogenic pulmonary edema
internal_medicine step2 -
Cardiac enzymes: When is measurement of cardiac enzymes the appropriate next step?
- When acute coronary syndrome is suspected (eg, ischemic ECG changes)
internal_medicine step2 -
Chest tube: When is placement of a chest tube indicated in acute respiratory presentation?
- For large pneumothorax or sustained pleural fluid causing respiratory compromise, not for PE
surgery internal_medicine step2 -
Steroids: When is IV hydrocortisone appropriate in acute dyspnea?
- For severe bronchospasm/asthma or adrenal crisis, not for PE without those features
internal_medicine pulmonology step2 -
ECG/clinical features: What ECG and clinical findings are typical but nonspecific for PE?
- Sinus tachycardia and acute dyspnea; ECG often otherwise nonspecific
internal_medicine step2 -
Imaging supplement: Show chest x-ray image associated with the case (illustration only).
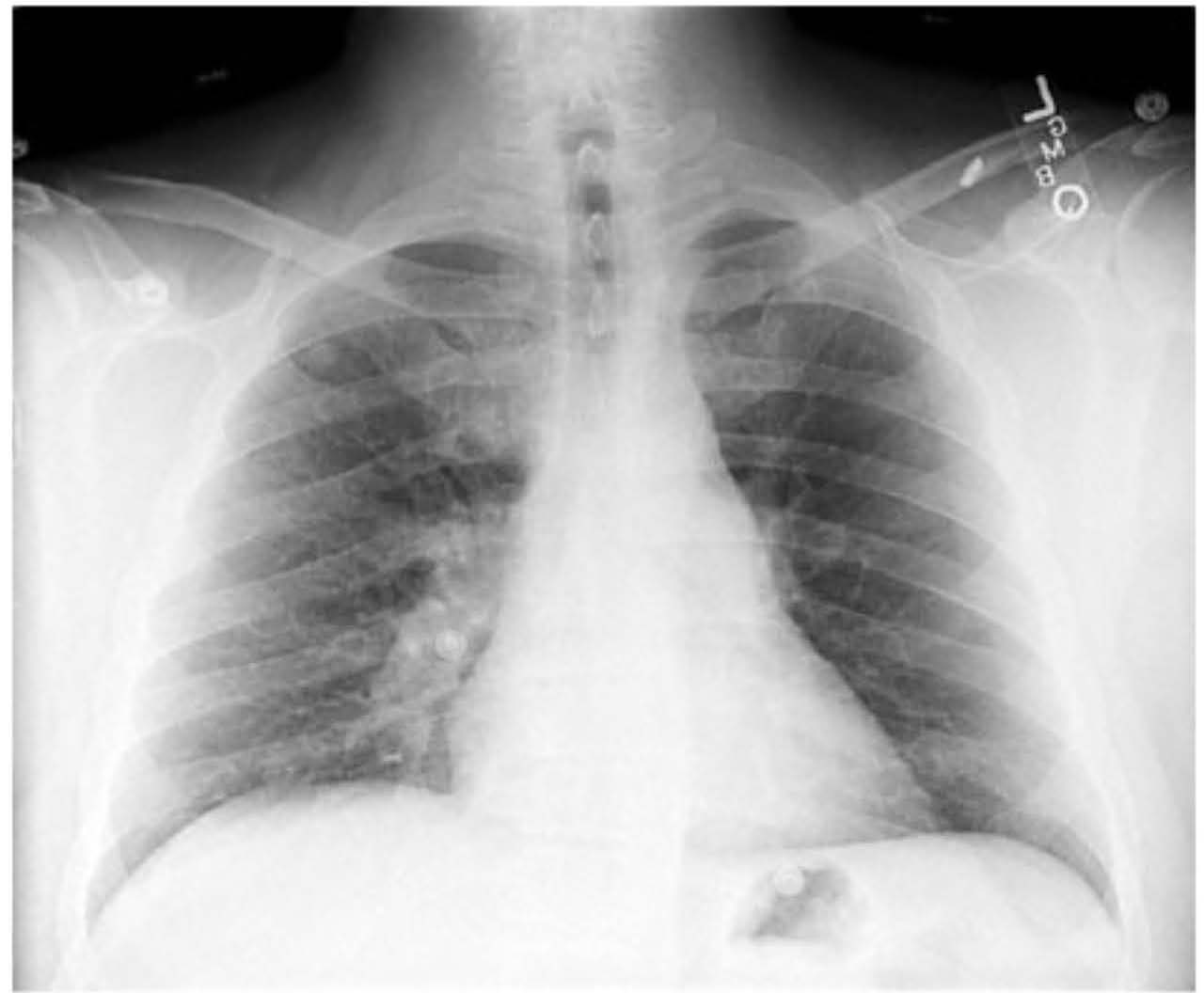 - Chest x-ray provided as supportive image; chest x-ray alone does not confirm PEinternal_medicine radiology step2
- Chest x-ray provided as supportive image; chest x-ray alone does not confirm PEinternal_medicine radiology step2 -
internal_medicine step2
-
Pulmonary embolism: clinical risk factors that prompt rapid testing (group 1)?
- Immobility
- Recent surgery
- Trauma / long-bone fracture
internal_medicine step2 -
Pulmonary embolism: additional clinical risk factors (group 2)?
- Obesity
- Malignancy
- Pregnancy or OCP use
internal_medicine step2 -
Diagnostic test: preferred method to confirm pulmonary embolism?
- Spiral CT scan of the chest (CT pulmonary angiography)
internal_medicine step2 -
D-dimer: limitation when Wells score indicates high pretest probability?
- Negative D-dimer may be false negative; CT angio required
internal_medicine step2 -
Obstructive shock from massive pulmonary embolism: best immediate management principle?
- Remove obstruction: thrombectomy or thrombolysis
internal_medicine step2 -
Hydrocortisone IV: when is it appropriate?
- COPD exacerbation causing SOB
- Hypotension refractory to fluids + vasopressors (suspect adrenal insufficiency)
internal_medicine step2 -
Hydrocortisone IV: why not appropriate for this patient with suspected PE?
- Patient lacks adrenal insufficiency or fluid-refractory hypotension; PE causes obstructive shock not responsive to vasopressors alone
internal_medicine step2 -
internal_medicine step2
-
Chest tube placement: why not appropriate for this patient?
- Patient chest x-ray lacks pleural effusion, hemothorax, pneumothorax
 internal_medicine step2
internal_medicine step2 -
Educational rule: when to test rapidly for pulmonary embolism?
- Sudden SOB with risk factors (immobility, surgery, malignancy, pregnancy/OCP, trauma/fracture, thrombophilia) → rapid diagnostic testing
internal_medicine step2 -
Clinical anchor: 82-year-old man with urinary retention (1700 mL turbid urine), hypotension unresponsive to fluids and norepinephrine, leukocytosis, hyponatremia, hyperkalemia, elevated BUN/Cr — what is the most likely endocrine contributor to persistent hypotension?
Adrenal insufficiency
internalmedicine step2. -
Clinical anchor: Which laboratory pattern in this patient supports adrenal insufficiency as a contributor to shock?
- Hyponatremia
- Hyperkalemia (borderline)
- Elevated BUN/Cr
internalmedicine step2. -
Clinical anchor: What is the most appropriate immediate therapy for suspected adrenal insufficiency causing refractory septic hypotension?
Intravenous hydrocortisone (glucocorticoid) supplementation
internalmedicine step2. -
Clinical anchor: Why is hydrocortisone indicated for vasopressor-refractory septic shock?
Glucocorticoid supplementation restores adrenal hormones and improves vasopressor responsiveness in refractory septic hypotension
internalmedicine step2. -
Clinical anchor: When would bladder irrigation with amphotericin B be appropriate instead of hydrocortisone?
Localized urogenital fungal infection requiring topical therapy; not for septic shock or hypotension
internalmedicine step2. -
Clinical anchor: When is intravenous fluconazole appropriate in a septic patient?
Documented or strongly suspected systemic fungal infection sensitive to fluconazole; not for immediate reversal of hypotension
internalmedicine step2. -
Clinical anchor: When is intravenous metronidazole appropriate in an infected patient with hypotension?
For infections by anaerobic bacteria (eg, intra-abdominal, pelvic) as antimicrobial therapy; not a vasopressor or shock reversal agent
internalmedicine step2. -
Clinical anchor: When is immediate hemodialysis indicated for hypotension with elevated BUN/Cr?
Indications: refractory hyperkalemia, volume overload unresponsive to diuretics, or severe uremic complications; mild creatinine rise alone does not mandate emergent dialysis
internalmedicine nephrology step2. -
Clinical anchor: What acute urologic finding in this case likely precipitated the sepsis?
Urinary retention with 1700 mL turbid urine indicating obstructive retention and likely infected bladder/UTI
internalmedicine surgery step2. -
Clinical anchor: How does limited vasopressor responsiveness relate to endocrine causes of shock in sepsis?
Limited vasopressor response is a hallmark of endocrine contributions (eg, adrenal insufficiency) to septic shock
internalmedicine criticalcare step2. -
internalmedicine step2.
-
Acute adrenal insufficiency: next immediate management for persistent hypotension after large-volume IV fluids and vasopressors?
IV glucocorticoids (eg, IV hydrocortisone)
internal_medicine step2. -
Why is IV glucocorticoid therapy correct for acute adrenal insufficiency with refractory hypotension?
Restores cortisol effect when production or responsiveness is insufficient, reversing vasopressor-refractory hypotension
internal_medicine step2. -
Pathophysiology of acute adrenal insufficiency mentioned in the text?
Insufficient adrenal hormone production or reduced responsiveness to adrenal hormones
internal_medicine step2. -
Indications for immediate hemodialysis per the text (group 1 of examples)?
- Life-threatening acidosis (eg, pH <6.9)
- Severe electrolyte derangement (eg, K+ >6.5 mEq/L)
internal_medicine step2. -
Indications for immediate hemodialysis per the text (group 2 of examples)?
- BUN >100 mg/dL with symptoms (pericarditis/encephalopathy)
- Dialyzable toxic ingestion (eg, aspirin)
internal_medicine step2. -
Why is emergent hemodialysis NOT appropriate for this patient now?
Patient is producing urine and does not meet emergent dialysis criteria
internal_medicine step2. -
How should hemodynamic instability be managed relative to dialysis initiation?
Address hemodynamics first or in parallel with dialysis to avoid circulatory collapse
internal_medicine step2. -
When should you suspect acute adrenal insufficiency in a hypotensive patient?
When hypotension persists despite large-volume IV fluids and vasopressors
internal_medicine step2. -
Which clinical action is emphasized as more appropriate than starting antibiotics for this patient's hypotension?
Treat suspected acute adrenal insufficiency with IV glucocorticoids rather than prioritizing empiric antibiotics
internal_medicine step2. -
Illustration: Slide showing highlighted teaching point about management of refractory hypotension — what does the image supplement?
Visual emphasis that IV glucocorticoids are the immediate step for adrenal insufficiency; image:
 internal_medicine step2.
internal_medicine step2. -
internalmedicine oncology step2.
-
internalmedicine oncology step2.
-
internalmedicine pathology step2.
-
Hodgkin lymphoma: required biopsy type for definitive diagnosis?
- Core-needle or excisional lymph node biopsy
internalmedicine surgery step2. -
Fine-needle aspiration (FNA): when is it appropriate for suspected lymphoma?
- Not appropriate for initial lymphoma diagnosis; use core/excisional when architecture needed
internalmedicine oncology step2. -
After Hodgkin lymphoma confirmation by node biopsy: next best staging test?
- PET scan (or contrast CT) to evaluate disease extent
internalmedicine oncology step2. -
Bronchoscopy: when is it indicated in suspected Hodgkin lymphoma?
- Indicated to biopsy intrathoracic pulmonary lesions seen on imaging, not for staging after node diagnosis
internalmedicine pulmonology step2. -
Laparoscopy: role in Hodgkin lymphoma evaluation?
- Not routine; consider only if liver biopsy required and no accessible lymph nodes
internalmedicine surgery step2. -
Pel-Ebstein fever: characteristic pattern in Hodgkin lymphoma?
- Recurrent high fevers 1–2 wk on, 1–2 wk off
internalmedicine infectiousdisease step2. -
Alcohol-induced lymph node pain: significance in Hodgkin lymphoma?
- Specific sign of Hodgkin disease-associated lymphadenopathy
internalmedicine oncology step2. -
internalmedicine laboratory step2.
-
Primary curative treatment approach for Hodgkin lymphoma?
- Chemotherapy often with concurrent radiation depending on location/bulk
internalmedicine oncology step2. -
Prognosis and staging uniqueness of Hodgkin lymphoma?
- Staged differently than other lymphomas and typically favorable prognosis
internalmedicine oncology step2. -
Diagnosis confirmation: what finding on lymph node biopsy confirms the diagnosis?
- Reed-Sternberg cells on core needle or excisional lymph node biopsy
internal_medicine step2 -
internal_medicine step2
-
internal_medicine step2
-
Treatment approach: what therapy is often curative for localized or bulky disease?
- Chemotherapy with concurrent radiation therapy depending on location and bulkiness
internal_medicine step2 -
Imaging example: what scans are shown for extent evaluation (illustration)?
- CT with contrast or PET scan illustrated
 internal_medicine step2
internal_medicine step2 -
Diagnosis: 67-year-old with sudden substernal chest pain, troponin ↑, hypotension, ST elevation in II, III, aVF and V4R–V6R. What is the most likely diagnosis?
- Inferior STEMI with right ventricular infarction
internal step2. -
ECG localization: Which ST-elevation leads indicate an inferior myocardial infarction and which indicate right ventricular involvement?
- Inferior MI: leads II, III, aVF
- Right ventricular infarct: leads V4R–V6R
internal step2. -
Hemodynamics: What does a laterally displaced point of maximal impulse and clear lungs suggest in this patient?
- Left ventricular enlargement/dysfunction with absence of pulmonary edema
internal step2. -
Central venous pressure: What CVP value is recorded and is it within normal range?
- CVP = 6 cm H2O; normal range 5–8 cm H2O
internal step2. -
Management anchor: For right ventricular infarction causing cardiogenic shock, what is the most appropriate initial step?
- IV crystalloid bolus (eg, 0.9% saline) to increase preload
internal step2. -
Why is IV furosemide incorrect as initial therapy for right ventricular infarction with hypotension?
- Diuretics decrease preload; right ventricular infarct patients are preload-dependent → worsens hypotension
internal step2. -
When is IV dobutamine appropriate in cardiogenic shock from right ventricular infarction?
- If shock persists after adequate fluid resuscitation; dobutamine increases contractility
internal step2. -
Why is IV propranolol contraindicated acutely in this hypotensive STEMI patient?
- Nonselective β-blocker (β1/β2) decreases contractility and heart rate → worsens hemodynamic instability
internal step2. -
Initial STEMI care bundle (besides fluids for RV infarct): Which immediate therapies should be given?
- Antiplatelet agents (eg, aspirin, clopidogrel)
- Anticoagulant (eg, heparin)
- Pain control + urgent coronary revascularization
internal step2. -
Why is pulmonary artery catheterization listed as an incorrect initial step in this scenario?
- PA catheterization is not the immediate stabilization step; initial management prioritizes fluids and urgent reperfusion
internal step2. -
Illustration: ECG pattern of inferior STEMI with right ventricular involvement — what leads to check for right ventricular ST elevation? (see image)
- Check right-sided precordial leads V4R–V6R for right ventricular ST elevation
 internal step2.
internal step2. -
ST-elevation myocardial infarction (STEMI): what is its urgency and classic acute presentation?
- True emergency
- Exertional substernal chest pressure
- Dyspnea, diaphoresis, nausea
- Typical patient has risk factors
internal_medicine cardiology step2. -
internal_medicine cardiology step2.
-
STEMI: what ECG finding confirms localization?
- ST-segment elevation in a specific vascular distribution
 internal_medicine cardiology step2.
internal_medicine cardiology step2. -
internal_medicine cardiology step2.
-
internal_medicine cardiology step2.
-
Right ventricular infarction: how does preload status affect initial stabilization?
- Preload-dependent → give intravenous crystalloids (eg, saline) as part of initial stabilization
internal_medicine cardiology step2. -
Administration of propranolol in a hypotensive patient: likely effect on cardiac output and blood pressure?
- Propranolol would decrease cardiac output and worsen hypotension
internal_medicine pharmacology step2. -
Pulmonary artery catheterization (PAC): when is PAC appropriate in shock?
- Useful for undifferentiated shock to assess hemodynamics
internal_medicine criticalcare step2. -
Pulmonary artery catheterization: why is PAC inappropriate when the shock cause is clear?
- Delaying treatment for PAC is inappropriate and potentially harmful when cause of shock is evident
internal_medicine criticalcare step2. -
Isoimmunization to the Kell erythrocyte antibody: strongest predisposing risk factor in this patient?
- History of blood transfusion
obgyn internal_medicine step2. -
Why is prior blood transfusion the strongest risk factor for Kell isoimmunization?
- Greater exposure to foreign RBC antigens; likelihood of isoimmunization rises with amount of blood exposed
obgyn internal_medicine step2. -
Pathophysiology: how do maternal anti-Kell antibodies affect the fetus?
- Maternal IgG antibodies cross placenta → hemolysis of fetal RBCs → fetal hemolytic anemia (eg, erythroblastosis fetalis)
pediatrics obgyn step2. -
How to determine fetal risk for Kell-related hemolysis when mother is anti-Kell positive?
- Determine paternal Kell antigen status; if father Kell-negative → fetus Kell-negative → no risk
obgyn internal_medicine step2. -
When is previous spontaneous abortion a significant risk for RBC isoimmunization?
- When fetal blood exposure occurred during passage of products of conception; it can cause alloimmunization but less than major transfusion exposure
obgyn internal_medicine step2. -
Why does maternal ABO blood group not increase risk for Kell isoimmunization?
- ABO type does not predispose to formation of anti-Kell antibodies
obgyn internal_medicine step2. -
Does Rho(D) immune globulin (RhoGAM) prevent Kell isoimmunization?
- No; RhoGAM decreases Rh(D) isoimmunization but does not prevent anti-Kell formation
obgyn internal_medicine step2. -
Is threatened abortion a strong risk factor for Kell isoimmunization?
- No; threatened abortion (scant bleeding with closed os) is less likely to cause significant fetal blood exposure compared with transfusion or completed abortion
obgyn internal_medicine step2. -
Comparison: blood transfusion vs spontaneous abortion as sources of maternal alloimmunization
- Transfusion: large antigen exposure → higher risk
- Spontaneous abortion: smaller exposure → lower risk (but still possible)
obgyn internal_medicine step2. -
Clinical step: how to assess fetal Kell antigen status when mother is anti-Kell positive (illustration)?
- Check paternal Kell status; if father Kell-positive → fetus may be Kell-positive → risk

obgyn pediatrics step2. - Check paternal Kell status; if father Kell-positive → fetus may be Kell-positive → risk
-
Rh(D) immune globulin: What is the mechanism preventing maternal alloimmunization?
Binds to Rh(D)-positive fetal cells in maternal circulation, preventing maternal immune system from forming anti-Rh(D) antibodies.
obgyn step2. -
Rh(D) immune globulin: Does it prevent maternal antibodies to Kell antigens?
No. Rh(D) immune globulin has no role against Kell antigens and does not change risk of Kell isoimmunization.
obgyn step2. -
Threatened abortion: What is the clinical definition?
Vaginal bleeding before 20 weeks with fetal cardiac activity present and closed cervical os.
obgyn step2. -
Threatened abortion: How does it affect risk of fetal erythrocyte isoimmunization?
It is a risk factor due to fetal–maternal blood mixing but exposes mother to a smaller blood volume than transfusion, so risk is less significant.
obgyn step2. -
Maternal alloimmunization: What exposures can lead to antibody formation?
- Blood transfusion
- Exposure to fetal blood antigens during delivery
internal_medicine step2. -
Alloimmunization risk: What determines likelihood of maternal isoimmunization?
Directly related to the amount of foreign blood exposure (greater exposure → higher likelihood).
internal_medicine step2. -
Fetal consequences: What are major risks from maternal red blood cell alloimmunization?
- Hemolytic anemia
- Erythroblastosis fetalis
- Death
pediatrics obgyn step2. -
When would threatened abortion be the primary concern for isoimmunization risk?
When fetal–maternal bleeding occurs before 20 weeks with fetal cardiac activity and closed os; it raises risk but is less significant than transfusion-level exposure.
obgyn step2. -
Alloimmunization overview: What summary rule links exposures and fetal risk?
Maternal antibodies form after transfusion or fetal blood exposure; magnitude of exposure predicts isoimmunization risk and fetal hemolytic complications.
internal_medicine obgyn step2. -
Illustration: What are the key fetal risks from maternal alloimmunization? (see image)
Key fetal risks: - Hemolytic anemia - Erythroblastosis fetalis - Death
 pediatrics obgyn step2.
pediatrics obgyn step2. -
Clinical decision: Safe discharge planning for a 92-year-old with acute confusion and poor memory — what is the primary priority?
- Patient safety: ensure safe living environment before discharge
internal_medicine step2. -
Clinical finding: 92-year-old with zero of three-word recall after 5 minutes — what does this suggest about capacity?
- Significant cognitive deficit: likely impaired capacity for independent living
neurology step2. -
Management decision: When is involving social services indicated in discharge planning?
- When patient lacks cognitive ability for self-care; arrange supervised living placement
internal_medicine step2. -
Correct answer rationale: Why is 'arrange placement in a supervised living facility' appropriate here?
- Patient has infections treated, hallucinations resolved, but persistent memory impairment → unsafe to live alone → social services to arrange supervised care
psychiatry step2. -
Option 'Bioethics: futile medical treatment' — when would this be appropriate?
- Appropriate when ongoing treatments provide no meaningful benefit or are medically futile
internal_medicine step2. -
Why is 'palliative care to discuss end-of-life planning' NOT appropriate for this patient now?
- No evidence of terminal/futile illness; current infections improving; immediate need is safe discharge planning, not end-of-life care
palliative step2. -
When would 'psychiatry to address an advance directive' be appropriate?
- Appropriate when assessing decision-making capacity for advance directives or identifying a medical power of attorney
psychiatry step2. -
Why is 'volunteer canine therapy' insufficient as the next step in discharge planning?
- Canine therapy may comfort the patient but does not address unsafe home environment or need for supervised placement
internal_medicine step2. -
Clinical anchor: Features of this patient's acute presentation that indicate delirium rather than chronic dementia
- Acute onset: found lethargic, new agitation/confusion, visual hallucinations that later resolved after treatment
neurology step2. -
Illustration: Slide showing highlighted discharge-planning teaching point — what role does social services play?
- Arrange supervised living for patients with cognitive deficits; see image for emphasis
 internal_medicine step2.
internal_medicine step2. -
Discharge planning: When are social services likely required for a patient?
- When a patient is unable to care for self, especially with no family involvement or help
internalmed step2. -
Discharge planning: What is the benefit of early social services involvement in the clinical course?
- Helps establish an optimum safe-discharge plan
internalmed step2. -
Define amaurosis fugax (clinical anchor).
Brief, transient, unilateral, painless vision loss due to retinal ischemia from microembolization of the ophthalmic artery.
neurology internalmedicine step2 -
Describe Hollenhorst plaque appearance and typical location (retinal finding).
- Yellow, refractile cholesterol embolus
- Located within retinal arterioles, often at arteriolar bifurcations
neurology internalmedicine step2 -
Primary source of emboli causing Hollenhorst plaques (diagnostic anchor).
Ipsilateral carotid arteries are the majority source of emboli causing retinal cholesterol plaques.
neurology internalmedicine step2 -
Most appropriate next diagnostic step for amaurosis fugax with Hollenhorst plaque (clinical decision).
Carotid duplex ultrasonography to evaluate for carotid atherosclerotic/ulcerative plaque.
neurology internalmedicine step2 -
When is echocardiography the preferred test for suspected retinal embolic source (choice C context)?
When emboli originate from calcific valvular plaques or intracardiac thrombus; calcific retinal emboli are chalky white and nonrefractile.
cardiology internalmedicine step2 -
When is cerebral MR angiography or brain MRI useful vs retinal embolic disease (choice B/E context)?
Useful to diagnose ischemic stroke or intracranial vascular lesions but unlikely to find the extracranial carotid source of retinal emboli.
neurology internalmedicine step2 -
Role of intraocular pressure measurement in acute vision loss workup (choice D context).
Measurement of intraocular pressure is important for glaucoma evaluation, not for diagnosing embolic retinal ischemia causing amaurosis fugax.
ophthalmology internalmedicine step2 -
How can treating carotid or cardiac valvular disease affect retinal/cerebral outcomes (management anchor)?
Treatment of carotid vascular or cardiac valvular disease can prevent central retinal artery occlusion and stroke.
neurology internalmedicine step2 -
Fundus photo: what finding supports carotid-source cholesterol embolus? (use image on answer for illustration)
Yellow, refractile plaques in retinal arterioles (Hollenhorst plaques) suggest carotid atheroembolism.
 neurology internalmedicine step2
neurology internalmedicine step2 -
Amaurosis fugax: defining clinical feature?
- Brief, transient, unilateral vision loss
- Indicative of retinal ischemia from emboli
neurology internalmedicine step2. -
Hollenhorst plaque: description
- Yellow, refractile, cholesterol embolus visible in retinal arterioles
ophthalmology internalmedicine step2. -
Amaurosis fugax: immediate diagnostic study
- Emergent carotid duplex ultrasonography to evaluate source (usually ipsilateral carotid artery)
surgery internalmedicine step2. -
Glaucoma: typical clinical course and key sign
- Insidious, chronic course with progressive peripheral vision loss
- Hallmark: cupping of the optic disc
ophthalmology internalmedicine step2. -
Why glaucoma is unlikely for brief transient vision-loss episodes?
- Glaucoma causes chronic progressive peripheral loss, not brief transient episodes (amaurosis fugax)
ophthalmology internalmedicine step2. -
Serum antinuclear antibody (ANA) assay: appropriate use
- Useful to evaluate systemic autoimmune disorders (eg, systemic lupus erythematosus)
rheumatology internalmedicine step2. -
Autoimmune vasculitis causing retinal/ophthalmic ischemia: typical vision-loss pattern
- Vision loss is acute or subacute and progressive, not transient/episodic
rheumatology internalmedicine step2. -
Giant cell arteritis (GCA): relation to amaurosis fugax and testing
- GCA may present with amaurosis fugax
- ANA assay is insufficient; erythrocyte sedimentation rate (ESR) is commonly associated biomarker
rheumatology internalmedicine step2. -
Amaurosis fugax management: source most commonly evaluated where?
- Evaluate ipsilateral carotid artery as most common embolic source
surgery internalmedicine step2. -
Fundus finding and embolus correlation (visual aid)
- Fundus exam may show retinal embolus (Hollenhorst plaque)
 ophthalmology neurology step2.
ophthalmology neurology step2. -
What is the most likely diagnosis for a 47-year-old with 3 months of weight loss, epigastric fullness, painless hyperbilirubinemia, mild ALP/AST/ALT elevation, and 30-year smoking history?
Pancreatic cancer
internal_medicine surgery step2. -
internal_medicine surgery step2.
-
Why is CT abdomen with contrast preferred for suspected pancreatic cancer?
CT with contrast best evaluates pancreatic mass extent and metastases to guide resectability
internal_medicine surgery step2. -
What laboratory pattern indicates cholestasis in this case?
Elevated total bilirubin (6 mg/dL) with increased alkaline phosphatase
internal_medicine step2. -
Which clinical features are classic for pancreatic head carcinoma?
- Painless jaundice
- Unintended weight loss
- Epigastric fullness/mass
internal_medicine surgery step2. -
surgery internal_medicine step2.
-
When is a bone scan appropriate in oncology?
Bone scan for osteoblastic bone metastases (eg, prostate, breast)
internal_medicine step2. -
When are flat and upright abdominal x-rays useful?
Detect bowel obstruction (air-fluid levels) or free air from perforation
internal_medicine step2. -
When is a HIDA scan indicated?
HIDA scan for acute cholecystitis, gallbladder emptying dysfunction, cholelithiasis with cystic duct obstruction
internal_medicine step2. -
Which risk factors for pancreatic cancer are listed in the case text?
- Smoking
- Obesity
- Chronic pancreatitis
internal_medicine step2. -
internal_medicine surgery step2
-
internal_medicine step2
-
internal_medicine step2
-
radiology internal_medicine step2
-
surgery internal_medicine step2
-
Right upper quadrant ultrasonography: primary clinical use?
- Evaluate liver and gallbladder pathologies
radiology internal_medicine step2 -
Right upper quadrant ultrasonography: when might it show an enlarged gallbladder in pancreatic disease?
- If a pancreatic head mass restricts biliary outflow
radiology surgery step2 -
Mild alkaline phosphatase, ALT, AST elevations in suspected pancreatic cancer: next best diagnostic step?
- CT scan of the abdomen with contrast
internal_medicine radiology step2 -
Choice E (RUQ ultrasonography) vs CT abdomen with contrast: when is CT preferred?
- CT abdomen with contrast preferred for evaluating suspected pancreatic cancer
internal_medicine radiology step2 -
Right upper quadrant ultrasonography: when is RUQ US the correct initial test?
- When evaluating liver or gallbladder pathology (eg, cholecystitis, gallstones)
internal_medicine step2 -
Define heat stroke (core features)
- Hyperthermia with environmental heat exposure
- Neurologic dysfunction (eg, altered mental status to obtundation)
- Cardiovascular instability (eg, tachypnea, hypotension)
internal_medicine neurology step2. -
Distinguish heat stroke from heat exhaustion
- Heat stroke: neurologic symptoms present
- Heat exhaustion: similar signs but neurologic exam intact
internal_medicine step2. -
Primary pathophysiology of heat stroke causing organ injury
- Excessive core temperature → cardiovascular and neurologic dysfunction → peripheral vasodilation → tissue ischemia and multi-organ failure
internal_medicine step2. -
Laboratory abnormalities associated with heat stroke
- Hypernatremia, hyperchloremia, hyperkalemia
- ↑ BUN, creatinine, creatine kinase
internal_medicine step2. -
Initial management priorities for heat stroke
- Rapid cooling (fans or ice water) and continuous core temperature monitoring
- Support airway, breathing, circulation
internal_medicine emergency step2. -
Why is evaporative cooling the correct immediate therapy for environmental heat stroke?
- Directly reduces core temperature quickly and addresses underlying hyperthermia; paired with ABCs and core temp monitoring
internal_medicine step2. -
When is CT scan of the head appropriate in altered mental status?
- For suspected ischemic or hemorrhagic stroke to guide interventions (eg, tPA) or structural causes
neurology internal_medicine step2. -
When is norepinephrine indicated for hypotension in heat stroke?
- After fluid resuscitation if hypotension persists; vasopressors support BP but do not treat hyperthermia
internal_medicine step2. -
When is dantrolene the correct therapy (contrast with heat stroke)?
- Treats neuroleptic malignant syndrome or malignant hyperthermia from drugs/anesthesia; not indicated for environmental heat stroke
psychiatry internal_medicine step2. -
When is lumbar puncture appropriate in altered mental status?
- When central nervous system infection (eg, meningitis) is suspected and imaging allows safe LP; not for isolated heat stroke
internal_medicine neurology step2. -
emergency internal_medicine step2.
-
Supportive steps during cooling for heat stroke (monitoring)
- Continuous core temperature monitoring
- Airway management and circulatory support (IV fluids first for hypovolemia)
internal_medicine step2. -
Illustration: evaporative cooling slide (supplement)
See image for a slide illustration of cooling measures:
 internal_medicine emergency step2.
internal_medicine emergency step2. -
Heat stroke: core definition and immediate pathophysiology?
- Heat stroke: failure of thermoregulation due to high environmental heat/humidity causing uncontrolled hyperthermia and multi-organ dysfunction
internalmedicine emergency step2. -
Heat stroke: cardinal vital-sign and systemic features?
- Features: hyperthermia, tachycardia, tachypnea, hypotension, neurologic dysfunction
emergency internalmedicine step2. -
Heat stroke: major complications to anticipate?
- Complications: shock; rhabdomyolysis; disseminated intravascular coagulation (DIC)
internalmedicine emergency step2. -
Heat stroke: initial management priorities?
- Treatment: active cooling (fans or ice-water), continuous core-temperature monitoring, support airway/breathing/circulation
emergency internalmedicine step2. -
Bacterial meningitis: typical presenting symptoms?
- Symptoms: fever; severe headache; neck stiffness; altered mental status or obtundation
neurology infectiousdisease step2. -
Cerebrospinal fluid (CSF) profile in bacterial meningitis?
- CSF: ↑ leukocytes with neutrophil predominance; ↑ protein; ↓ glucose
neurology infectiousdisease step2. -
Lumbar puncture (LP): when is it useful?
- LP: useful for diagnosing meningitis and other infectious/inflammatory CNS disorders
neurology internalmedicine step2. -
Clinical distinction: heat stroke vs bacterial meningitis—key discriminating history?
- Distinguishing feature: recent exposure to extreme environmental heat favors heat stroke over meningitis
emergency internalmedicine step2. -
Why LP is less appropriate for patient with hyperthermia after heat exposure?
- Reason: hyperthermia from extreme environmental heat provides a more likely cause than meningitis, so LP is less indicated
internalmedicine emergency step2. -
Heat stroke: monitoring and support measures during treatment (supplemental image)?
- Monitor/support: continuous core-temperature monitoring; airway/breathing/circulation support
 emergency internalmedicine step2.
emergency internalmedicine step2. -
Phentermine: mechanism causing hypertension?
- Increases norepinephrine release → α-adrenergic vasoconstriction
psychiatry pediatrics step2. -
Hypertensive emergency: diagnostic threshold and requirement?
- BP > 180/120 mm Hg plus end-organ damage
internal_medicine neurology step2. -
Common presenting symptoms of sympathomimetic-induced hypertensive emergency?
- Headache
- Epistaxis
- Neurologic deficits
neurology pediatrics step2. -
Clinical features in the presented 15-year-old phentermine overdose case?
- Severe headache, chest pain
- BP 220/125 mm Hg, pulse 55/min, generalized hyperreflexia
pediatrics internal_medicine step2. -
Sodium nitroprusside: clinical role in sympathomimetic hypertensive emergency?
- Immediate IV vasodilator to reverse α-mediated vasoconstriction and lower BP
internal_medicine emergency step2. -
Sodium nitroprusside: described mechanism of action (as stated)?
- Releases nitrous oxide and acts as arterial and venodilator
internal_medicine step2. -
Phentolamine: role in sympathomimetic hypertensive emergency?
- α-adrenergic blocker option to treat catecholamine-mediated hypertension
internal_medicine step2. -
internal_medicine step2.
-
IV furosemide: when is it appropriate for hypertension?
- Diuresis for heart failure, cirrhosis, kidney disease; not for acute sympathomimetic vasoconstriction
internal_medicine step2. -
IV phenytoin: appropriate emergent indications?
- Status epilepticus and other seizures via Na+ channel blockade; not for hypertension
neurology step2. -
IV physostigmine: correct emergent indication?
- Anticholinergic toxicity reversal; not used for hypertensive emergency
psychiatry internal_medicine step2. -
IV verapamil: contraindication present in this case?
- Bradycardia present (pulse 55/min) → verapamil contraindicated due to AV conduction worsening
cardiology internal_medicine step2. -
Endotracheal intubation: indications relevant to this patient?
- Indicated for airway protection, apnea, hypoxemia, hypercarbia; not indicated here (no respiratory failure)
surgery pediatrics step2. -
Comparison: sodium nitroprusside versus verapamil in this overdose scenario?
- SNP: immediate arterial + venous vasodilation for severe hypertension
- Verapamil: slows AV node, contraindicated with bradycardia
cardiology internal_medicine step2. -
Sodium nitroprusside: illustration of use (slide image)?
- Use in sympathomimetic hypertensive emergency
 internal_medicine step2.
internal_medicine step2. -
internal_medicine step2
-
Phentermine: which vascular effect is counteracted by intravenous sodium nitroprusside?
- Vasoconstriction
internal_medicine step2 -
Atrial septal defect (ASD): key auscultatory findings?
- Fixed, widely split S2
- Grade 3/6 midsystolic murmur at 2nd left intercostal space
internal_medicine step2. -
Atrial septal defect (ASD): primary pathophysiology?
- Left-to-right atrial shunt → RA/RV volume overload → increased RV stroke volume
internal_medicine cardiology step2. -
Why does ASD cause a fixed, widely split S2?
- RV volume overload → delayed pulmonic valve closure → persistent wide split S2
internal_medicine cardiology step2. -
Uncorrected ASD: most important long-term complication?
- Pulmonary arterial hypertension from pulmonary vascular remodeling → possible shunt reversal (Eisenmenger) and cyanosis
internal_medicine cardiology step2. -
Why is pulmonary hypertension the correct long-term risk in ASD?
- Chronic left-to-right shunt increases pulmonary flow/pressure → pulmonary vascular remodeling → pulmonary arterial hypertension
internal_medicine cardiology step2. -
Cholestasis: typical cause and presentation?
- Cause: biliary obstruction (eg, pancreatic head tumor)
- Presentation: painless jaundice, anorexia
internal_medicine gastroenterology step2. -
Why is cholestasis unlikely in this young woman with ASD?
- No evidence of intra-abdominal mass or painless jaundice; clinical exam normal
internal_medicine step2. -
Budd-Chiari syndrome (hepatic vein thrombosis): common risk factors?
- Hypercoagulable states: pregnancy, antiphospholipid syndrome, protein C deficiency, malignancy
internal_medicine hepatology step2. -
Why is Budd-Chiari unlikely in this patient despite OCP use?
- OCPs increase clot risk but patient lacks other hypercoagulable signs; no hepatic symptoms given
internal_medicine step2. -
Hepatitis: common causes and presentation?
- Causes: viral, medication-induced, autoimmune, alcoholic
- Presentation: transaminitis, jaundice, RUQ pain
internal_medicine infectious_disease step2. -
Why is acute hepatitis unlikely in this patient?
- No heavy alcohol use, no offending medications, and no high-risk behaviors or hepatic symptoms
internal_medicine step2. -
Renovascular hypertension from fibromuscular dysplasia: typical patient and exam?
- Young female; renal artery beading on angiography; possible abdominal bruit
internal_medicine nephrology step2. -
Why is renovascular hypertension unlikely in this patient?
- No abdominal bruit and no other signs suggesting renal artery stenosis or fibromuscular dysplasia
internal_medicine nephrology step2. -
internal_medicine cardiology step2.
-
Why is systemic hypertension unlikely in this 22-year-old woman?
- Lacks typical risk factors (young age, no heavy alcohol use, no high-sodium diet noted); BP normal at 100/70 mm Hg
internal_medicine cardiology step2. -
Eisenmenger syndrome: defining features and consequence?
- Shunt reversal from long-standing pulmonary hypertension → cyanosis and right-to-left shunt physiology
internal_medicine cardiology step2. -
Midsystolic ejection murmur in ASD: mechanism?
- Increased RV stroke volume across pulmonary valve → physiologic ejection murmur
internal_medicine cardiology step2. -
ASD subtypes: commonest type and association with ostium primum?
- Ostium secundum = most common
- Ostium primum associated with Down syndrome
pediatrics internal_medicine step2. -
Illustration: ASD pathophysiology and auscultation (supplemental image)
See illustration:
 — image supplements ASD flow and auscultatory findingsinternal_medicine cardiology step2.
— image supplements ASD flow and auscultatory findingsinternal_medicine cardiology step2. -
Atrial septal defect (ASD): primary pathophysiologic effect on the pulmonic valve?
Increased blood flow through the pulmonic valve
pediatrics internalmedicine step2. -
pediatrics internalmedicine step2.
-
Atrial septal defect (ASD): which defect type is commonly associated with Down syndrome?
Ostium primum defect
pediatrics internalmedicine step2. -
Atrial septal defect (ASD): severe complication from long-standing uncorrected defect?
- Pulmonary hypertension
- Eisenmenger syndrome with reversal of the left-to-right shunt
pediatrics internalmedicine step2. -
Bacterial vaginosis: defining clinical features in adolescent with vaginal discharge
- Gray, thin, malodorous vaginal discharge
- Mild pruritus
- Recent antibiotic use
obgyn pediatrics step2. -
Bacterial vaginosis: primary pathophysiology and common organism
- Shift in vaginal flora → bacterial overgrowth
- Most common: Gardnerella vaginalis (gram-variable coccobacilli)
obgyn internalmedicine step2. -
Clue cells: microscopic definition
- Epithelial cells coated with bacteria
- Appear granular with irregular margins on wet mount
obgyn pediatrics step2. -
Bacterial vaginosis: diagnostic lab findings
- Vaginal pH > 4.5
- Fishy odor on KOH (whiff) test
- Clue cells on wet mount
obgyn internalmedicine step2. -
obgyn internalmedicine step2.
-
Bacterial vaginosis: sexual transmission and partner treatment policy
- Not considered an STI
- Do not treat asymptomatic sexual partners
obgyn pediatrics step2. -
Antibiotic exposure: role in bacterial vaginosis development
- Antibiotics disrupt normal lactobacilli → predispose to BV
obgyn internalmedicine step2. -
Chemical irritation (bubble baths): typical genital findings vs discharge
- External vulvar erythema, dryness, pruritus, possible excoriations
- Unlikely to cause gray malodorous vaginal discharge or clue cells
obgyn pediatrics step2. -
Latex allergy (condom): typical genital findings vs vaginal discharge
- Vulvar erythema, itching, dermatitis
- Unlikely to produce internal gray malodorous discharge or clue cells
obgyn pediatrics step2. -
Physiologic vaginal secretions: distinguishing features from pathologic discharge
- Small amounts, clear or white, variable with cycle
- Not malodorous; no clue cells
obgyn pediatrics step2. -
Trichomoniasis: typical clinical features differentiating from BV
- Green, frothy, malodorous discharge
- Pruritus, dysuria, dyspareunia, cervical erythema (strawberry cervix)
obgyn infectiousdisease step2. -
Comparison: BV versus Trichomonas key distinguishing points
- BV: gray thin discharge, clue cells, pH >4.5, fishy KOH
- Trichomonas: green frothy discharge, dysuria, cervical erythema
obgyn internalmedicine step2. -
Bacterial vaginosis: supportive image of wet mount (clue cells)
- Clue cells on wet mount: epithelial cells coated with bacteria
 obgyn pediatrics step2.
obgyn pediatrics step2. -
Bacterial vaginosis: what organism causes the condition?
- Gardnerella vaginalis (gram-variable, facultative anaerobic coccobacilli)
obgyn internal step2 -
Bacterial vaginosis: describe the typical vaginal discharge.
- Gray, thin, malodorous vaginal discharge
obgyn internal step2 -
obgyn internal step2
-
Bacterial vaginosis: what is the potassium hydroxide (KOH) finding?
- Fish-like odor on KOH (positive whiff test)
obgyn internal step2 -
obgyn internal step2
-
obgyn internal step2
-
Bacterial vaginosis: is it considered a sexually transmitted infection (STI)?
- No; bacterial vaginosis is not considered an STI
obgyn internal step2 -
obgyn internal step2
-
What is pubertal gynecomastia?
- Benign proliferation of glandular breast tissue in boys aged 12–14, often SMR stage 3
pediatrics step2. -
What pathophysiologic mechanism causes pubertal gynecomastia?
- Relative androgen/estrogen imbalance from peripheral conversion of androstenedione and testosterone to estrone/estradiol
internal_medicine step2. -
Typical physical exam features of pubertal gynecomastia?
- Tender, firm, mobile subareolar mass (~1 cm)
pediatrics step2. -
What is the expected result of laboratory studies in physiologic pubertal gynecomastia?
- Normal laboratory studies
internal_medicine step2. -
Management of physiologic pubertal gynecomastia in an otherwise healthy adolescent?
- Reassurance; most self-resolve; medical/surgical options (eg, aromatase inhibitors, liposuction) for symptoms
pediatrics surgery step2. -
Why is 'Puberty' the most likely cause of the 14-year-old boy's breast swelling?
- Age 12–14 and SMR stage 3 correspond to physiologic gynecomastia from increased estrogen via peripheral aromatization
pediatrics step2. -
When would SSRI-associated gynecomastia be the correct diagnosis?
- If gynecomastia appears after SSRI use and alternative causes excluded; note SSRIs are not generally associated with gynecomastia
psychiatry step2. -
How does male breast cancer usually differ on exam from benign gynecomastia?
- Malignancy tends to be fixed (not mobile) due to invasive growth; less likely in adolescent boys
surgery step2. -
When is marijuana a likely cause of gynecomastia and by what proposed mechanism?
- With recurrent use; proposed disruption of hepatic estrogen metabolism by THC causing increased estrogen
internal_medicine step2. -
Which clinical features suggest Klinefelter syndrome (seminiferous tubule dysgenesis) rather than pubertal gynecomastia?
- Learning disabilities, testicular atrophy, tall stature with long extremities
pediatrics step2. -
Physical exam illustration: subareolar tender breast mass — what diagnosis does this support?
- **Supports pubertal gynecomastia when age/SMR fit; exam: tender, firm, mobile subareolar mass
 **pediatrics step2.
**pediatrics step2. -
Anchor: Initial diagnostic step for 47-year-old with 6-month progressive low back pain without neurologic deficits or red flags?
- X-ray series of the lumbar spine
internal step2. -
Anchor: Pathophysiology components of degenerative disc disease?
- Cartilaginous endplates
- Annulus fibrosus
- Nucleus pulposus
neurology step2. -
Anchor: Mechanism causing loss of disc height in degenerative disc disease?
- Decreased nutrient diffusion from endplates + decreased nucleus pulposus water content → loss of disc height
neurology step2. -
Anchor: How do annulus fibrosus tears develop in degenerative disc disease?
- Repetitive axial forces on dehydrated disc → annular tears
orthopedics step2. -
neurology step2.
-
Anchor: Typical pain features of degenerative disc disease?
- Worse with flexion, Valsalva, coughing, or sneezing
internal step2. -
Anchor: Physical exam tests and signs to evaluate for radiculopathy?
- Straight-leg raise (positive = reproduction of leg pain)
- Sensory deficits, DTR changes, muscle weakness
neurology step2. -
Anchor: Red-flag features indicating possible cauda equina or conus medullaris syndrome requiring emergent surgery?
- Saddle anesthesia
- Bowel/bladder incontinence
- Lower extremity weakness
surgery step2. -
Anchor: Indication for MRI of the lumbar spine in low back pain?
- Acute neurologic deterioration or signs of myelopathy (eg, cauda equina/conus medullaris)
neurology step2. -
Anchor: Appropriate use of bone scan in back pain?
- Characterize concerning osseous lesion or detect osteoblastic metastases (eg, prostate, breast)
oncology step2. -
Anchor: Role of CT myelography versus MRI in spine imaging?
- CT myelography used historically for spinal cord evaluation after intrathecal contrast; largely replaced by MRI (better accuracy, noninvasive, no radiation)
radiology step2. -
Anchor: Conservative treatments for degenerative disc disease?
- NSAIDs
- Hot/cold compress, weight loss, activity modification, physical therapy
internal step2. -
Anchor: When to obtain initial imaging for low back pain?
- Initial imaging (x-ray) indicated for chronic pain without neurologic deficits or trauma to evaluate degenerative changes
internal step2. -
Anchor: Supplementary slide showing recommended initial test for chronic low back pain (image on answer)
Initial test: X-ray series of the lumbar spine
 internal step2.
internal step2. -
Cauda equina compression: core presenting features?
- Bilateral lower extremity weakness
- Abnormal deep tendon reflexes
- Bowel or bladder dysfunction
- Saddle anesthesia
neurology surgery step2. -
Cauda equina compression: common acute causes?
- Acute disc herniation
- Traumatic vertebral column fracture
- Pathologic vertebral fracture
neurology surgery step2. -
Initial imaging for suspected lumbar spine problem without neurologic deficits?
- Plain x-ray series of the lumbar spine
internal_medicine surgery step2. -
Role of MRI in acute lumbosacral compression when initial exam lacks deficits?
- MRI may be required later to guide therapy after plain x-rays
neurology radiology step2. -
Degenerative disc disease: primary pathophysiologic processes?
- Repetitive axial forces
- Decreased nutrient gradient
- Declining nucleus pulposus water content with aging
orthopedics internal_medicine step2. -
Degenerative disc disease: how annulus fibrosus tears form?
- Result from repetitive axial forces + declining nucleus pulposus hydration and nutrients
orthopedics surgery step2. -
Degenerative disc disease: typical symptom triggers?
- Pain worsens with flexion
- Pain with Valsalva, cough, or sneezing
internal_medicine neurology step2. -
Degenerative disc disease: first-line nonprocedural treatments (group 1)?
- NSAIDs
- Hot or cold compresses
internal_medicine pain step2. -
Degenerative disc disease: first-line nonprocedural treatments (group 2)?
- Weight loss
- Activity modification
- Physical therapy
internal_medicine rehabilitation step2. -
Imaging workflow for patient with lumbar complaint and no neurologic deficits: concise plan?
- Obtain plain x-rays first; consider MRI later if therapy guidance needed
radiology surgery step2. -
Supplemental image: presentation slide relevant to lumbar imaging and degenerative disc disease?
Slide image for review:
 radiology internal_medicine step2.
radiology internal_medicine step2. -
Membranous nephropathy: core nephrotic syndrome features?
- Proteinuria >3 g/day
- Edema
- Hypoalbuminemia
internal_medicine step2. -
Membranous nephropathy: key biopsy/immunofluorescence findings?
- Diffuse GBM thickening
- IgG along GBM (IF)
- Subepithelial electron-dense deposits
internal_medicine step2. -
internal_medicine step2.
-
Pathophysiology: why hypercholesterolemia occurs in nephrotic syndrome?
Liver increases lipoprotein synthesis to compensate for low serum oncotic pressure from urinary albumin losses
internal_medicine step2. -
ACE inhibitor therapy: mechanism slowing progression of membranous nephropathy?
ACE inhibitors ↓ angiotensin II → relative efferent arteriole dilation → ↓ glomerular filtration pressure → ↓ hyperfiltration injury
internal_medicine step2. -
Why is ACE inhibitor (eg, lisinopril) the correct choice for delaying renal progression in membranous nephropathy?
ACE inhibitor reduces intraglomerular pressure and hyperfiltration, delaying nephropathy progression
internal_medicine step2. -
High-protein diet: when would it be appropriate in kidney disease?
High-protein diet is not appropriate; kidney disease patients should generally avoid high protein to reduce glomerular injury
internal_medicine step2. -
High-potassium diet: when is it indicated in kidney disease?
High-potassium diet is inappropriate; patients with kidney disease generally should limit potassium
internal_medicine step2. -
Beta-blocker therapy (eg, metoprolol): when would it be preferred over ACE inhibitor for renal protection?
Beta-blockers treat arrhythmia/hypertension/CHF but do not reduce intraglomerular hyperfiltration and are not used to slow nephropathy progression
internal_medicine step2. -
Diuretic therapy: appropriate indication in membranous nephropathy?
Diuretics treat hypervolemia/edema; avoid if patient lacks volume overload because diuretics can reduce renal perfusion and worsen function
internal_medicine step2. -
Membranous nephropathy: summary preventive treatment principle for slowing progression?
Reduce intraglomerular pressure (eg, ACE inhibitors) to limit hyperfiltration injury
internal_medicine step2. -
Visual: membranous nephropathy features (illustration). What biopsy features are shown?
- Diffuse GBM thickening
- Subepithelial deposits (electron microscopy)
 internal_medicine step2.
internal_medicine step2. -
Osteoporosis trial result: what does a P-value of 0.047 indicate about chance?
P-value < 0.05 → result unlikely due to random chance
internal_medicine step2. -
Osteoporosis trial: how large was the absolute reduction in hip-fracture rate?
- 0.044 − 0.042 = 0.002 (0.2% absolute reduction)
internal_medicine step2. -
Why is the trial result statistically significant but not clinically significant?
Statistically significant (P<0.05) but absolute benefit only 0.2% → minimal individual benefit; NNT exceedingly high; unlikely to change practice or justify costs/risks
internal_medicine step2. -
When would 'results likely caused by chance' be a correct conclusion?
If P-value ≥ 0.05 (no statistical significance) → cannot exclude random chance
internal_medicine step2. -
Definition: placebo effect as described in the trial explanation
Beneficial effect from placebo due to patient belief, not from placebo's properties
internal_medicine step2. -
When could the placebo effect explain a trial difference?
When outcomes are subjective and patient belief can alter perceived benefit; not likely to explain objective fracture-rate reductions
internal_medicine step2. -
Why is 'inadequate power' unlikely for this osteoporosis trial?
Large sample: 19,916 participants over 3 years → study likely well powered to detect small differences
internal_medicine step2. -
What does 'clinical significance' require beyond statistical significance?
Benefit magnitude that alters practice and outweighs risks/costs
internal_medicine step2. -
Applicability: what does 'applicability' mean for a treatment effect?
Extent to which a study's observed treatment effect will reflect the effect in actual patients outside the study.
internalmedicine step2. -
Applicability: main factors that can affect whether study results apply to non-study patients?
- Similarity of baseline characteristics
- Demographics
- Clinical scenario and treatment
internalmedicine step2. -
Applicability example: elderly patient with osteoporosis on calcium and vitamin D — are study results likely applicable?
Yes; this patient closely reflects the elderly osteoporotic study population treated with calcium and vitamin D, so study results reasonably apply.
internalmedicine step2. -
Statistical power: what does 'power' describe?
Ability of a study to detect a difference between groups if one exists.
internalmedicine step2. -
Factors that may influence statistical power (small list)?
- Baseline incidence of outcome
- Population variance
- Magnitude of treatment effect
internalmedicine step2. -
When is 'inadequate power' a correct explanation for study findings?
When the study lacks ability to detect an existing difference (underpowered), making a true effect statistically undetected.
internalmedicine step2. -
Why is 'inadequate power' an incorrect explanation if the study was adequately powered?
Adequate power means the study could detect a difference; if a small-magnitude difference was found, inadequate power is not the cause.
internalmedicine step2. -
What does a conventional P-value cutoff of 0.05 indicate?
Result was unlikely to occur due to random chance (statistical significance threshold).
internalmedicine step2. -
How does statistical significance (P≤0.05) differ from clinical significance?
Statistical significance ≠ clinical significance; clinical significance requires likely change in practice and benefits that outweigh risks and costs.
internalmedicine step2. -
Study statement: Can power change the magnitude of an observed treatment effect?
No; power affects ability to detect a difference, not the magnitude of the detected difference.
internalmedicine step2. -
Visual: slide illustrating highlighted teaching points (useful as summary)
Illustration of applicability, power, and P-value concepts:
 internalmedicine step2.
internalmedicine step2. -
Define 'hematogenous osteomyelitis' in children (anchor: osteomyelitis presentation).
- Infection of bone/bone marrow from bloodstream causing pain, fever, inability to bear weight
pediatrics internalmedicine step2. -
Key clinical features of pediatric hematogenous osteomyelitis (anchor: clinical presentation).
- Fever
- Localized pain/tenderness
- Difficulty bearing weight or refusal to walk
pediatrics internalmedicine step2. -
Laboratory and imaging findings supporting osteomyelitis (anchor: diagnostics).
- Leukocytosis, elevated CRP
- MRI showing marrow edema
pediatrics internalmedicine step2. -
Most likely pathogen for hematogenous osteomyelitis in this 2-year-old (anchor: microbiology).
Staphylococcus aureus (most common cause in this age)
pediatrics infectiousdisease step2. -
Gram-stain clue pointing to Staphylococcus aureus (anchor: Gram stain interpretation).
Gram-positive cocci in clusters on blood culture Gram stain
pediatrics internalmedicine step2. -
First-line initial antibiotic choice for suspected MRSA/MSSA pediatric osteomyelitis (anchor: initial management).
Vancomycin (covers MRSA and MSSA pending sensitivities)
pediatrics infectiousdisease step2. -
Why ampicillin is inappropriate as initial monotherapy here (anchor: ampicillin limitation).
Ampicillin active vs some gram-positive/gram-negative but is not effective against MRSA
pediatrics internalmedicine step2. -
When would azithromycin be an appropriate choice (anchor: azithromycin spectrum)?
Macrolide primarily effective against some gram-positive organisms; not reliable for MRSA empiric therapy
pediatrics internalmedicine step2. -
Rationale for starting broad-spectrum therapy in suspected pediatric osteomyelitis (anchor: treatment principle).
Prompt broad antibiotics needed because hematogenous seeding can cause bacteremia and distant bone infection; tailor after culture sensitivities
pediatrics infectiousdisease step2. -
Other common pediatric osteomyelitis pathogens besides S. aureus (anchor: differential microbiology).
- Group A streptococci
- Streptococcus pneumoniae
- Haemophilus influenzae
pediatrics infectiousdisease step2. -
Why ceftriaxone/cefepime/rifampin were not chosen as initial therapy in this case (anchor: initial-choice logic).
Initial therapy must reliably cover MRSA; these agents do not reliably provide empiric MRSA coverage pending culture results
pediatrics internalmedicine step2. -
Osteomyelitis (pediatric): definition
Infection of bone and bone marrow; typically develops from hematogenous spread in children.
pediatrics infectious step2. -
pediatrics infectious step2.
-
Osteomyelitis (pediatric): other common bacteria (group 1)
- Streptococcus pyogenes (Group A streptococci)
- Streptococcus pneumoniae
pediatrics infectious step2. -
pediatrics infectious step2.
-
Initial antibiotic choice for suspected pediatric osteomyelitis with possible MRSA
Vancomycin — effective against MRSA and MSSA; appropriate initial therapy.
pediatrics internalmedicine step2. -
Why ceftriaxone or cefepime alone is NOT initial monotherapy for suspected MRSA osteomyelitis
Ceftriaxone/cefepime cover gram-positive and gram-negative bacteria but are not effective against MRSA.
pediatrics infectious step2. -
When is cefepime specifically useful in bone infection coverage?
Cefepime adds Pseudomonas coverage (unlike ceftriaxone).
pediatrics infectious step2. -
Role of combining vancomycin with ceftriaxone/cefepime in osteomyelitis
Combination may be used to broaden coverage (vancomycin for MRSA plus ceftriaxone/cefepime for gram-negatives).
pediatrics internalmedicine step2. -
Azithromycin in suspected MRSA osteomyelitis: appropriateness
Azithromycin is not effective against MRSA and is not appropriate as initial therapy for suspected MRSA osteomyelitis.
pediatrics infectious step2. -
Rifampin: mechanism and limits relevant to osteomyelitis
Rifampin inhibits bacterial RNA polymerase; active vs mycobacteria and some gram-positives but not effective as sole initial therapy for MRSA.
pediatrics infectious step2. -
Pathogenesis anchor: how pediatric osteomyelitis usually arises
Hematogenous seeding of bone and marrow in pediatric patients.
pediatrics surgery step2. -
Supplementary: slide image for osteomyelitis teaching (illustration only)
Supplementary figure illustrating teaching points.
 pediatrics internalmedicine step2.
pediatrics internalmedicine step2. -
Rheumatic mitral valve disease: what is the pathophysiology linking group A strep to progressive valve damage?
- Molecular mimicry after group A streptococcal infection → progressive inflammatory damage to valves → fibrosis and calcification
internal_medicine step2. cardiology -
Rheumatic fever: key extra-cardiac clinical findings
- Joint inflammation
- Subcutaneous nodules
- Erythema marginatum
- Sydenham chorea
internal_medicine step2. infectious -
Rheumatic mitral valve disease: typical acute vs chronic valve dysfunction
- Acute: mitral insufficiency
- Chronic (later): mitral stenosis
internal_medicine step2. cardiology -
Mitral stenosis: classic auscultatory and complication features
- Diastolic rumble at apex radiating to axilla
- Can cause left atrial enlargement, pulmonary edema, atrial fibrillation/flutter
internal_medicine step2. cardiology -
Why rheumatic mitral valve disease best explains this patient: 32-year-old with 6 months dyspnea, irregular tachycardia, holosystolic murmur and diastolic rumble at apex, AF, RVH?
- Mitral valve disease from rheumatic damage causes diastolic murmur at apex, LA enlargement → AF and pulmonary congestion; fits progressive rheumatic mitral stenosis
internal_medicine step2. cardiology -
Aortic stenosis from calcified tricuspid aortic valve: when is this the usual cause and typical findings?
- Common in elderly due to trileaflet calcification
- Symptoms: exertional syncope, angina, dyspnea
- Murmur: crescendo-decrescendo systolic at right upper sternal border
internal_medicine step2. surgery -
Bicuspid aortic valve calcification: typical patient group and mechanism
- Younger patients (than tricuspid) due to abnormal leaflet geometry → turbulent shear, earlier calcification
internal_medicine step2. pediatrics -
Atrial septal defect (ASD): hemodynamic effects and auscultatory clues when ASD is the correct diagnosis
- Left→right shunt → RA/RV volume overload, delayed pulmonic valve closure → fixed split S2 and low-grade ejection murmur
- Chronic → pulmonary HTN, possible Eisenmenger with cyanosis
internal_medicine step2. cardiology -
Ventricular septal defect (VSD): classic murmur and typical location heard
- Holosystolic murmur best heard at left lower sternal border
internal_medicine step2. pediatrics -
Infective endocarditis (Staphylococcus aureus or viridans): typical presenting features that support this diagnosis
- Fever
- New cardiac murmur
- Fatigue
- Septic embolic phenomena
internal_medicine step2. infectious -
Slide image: supporting visual summary of exam item (use as reference only)
 - Visual summary of rheumatic mitral disease, murmurs, ASD/VSD, aortic stenosis, and endocarditis featuresinternal_medicine step2. cardiology
- Visual summary of rheumatic mitral disease, murmurs, ASD/VSD, aortic stenosis, and endocarditis featuresinternal_medicine step2. cardiology -
internalmedicine cardiology step2
-
Mitral stenosis — classic auscultatory findings?
- Opening snap
- Diastolic rumble loudest at cardiac apex
internalmedicine cardiology step2 -
Cause: Long-term complication that classically produces mitral stenosis?
Rheumatic heart disease from group A streptococcal infections
internalmedicine infectiousdisease step2 -
Complications of severe mitral stenosis?
- Left atrial enlargement
- Cardiogenic pulmonary edema
- Atrial fibrillation/flutter
internalmedicine cardiology step2 -
Why is infective endocarditis unlikely for a patient with 6 months of symptoms?
Endocarditis usually presents acutely/subacutely; 6 months untreated would likely be fatal
internalmedicine infectiousdisease step2 -
When would endomyocarditis/myocarditis be the correct diagnosis?
In inflammatory or postviral syndromes with raised troponin, ECG changes, and possible heart-failure symptoms; presentation is typically acute
internalmedicine cardiology step2 -
Why is pericarditis an unlikely diagnosis for this patient?
Pericarditis causes sharp chest pain worse when supine, better sitting up; ECG shows diffuse ST elevation and PR depression; patient lacks these features and murmur/ECG are inconsistent
internalmedicine cardiology step2 -
Pericarditis — common causes and ECG pattern?
Causes: viral infection, SLE, tuberculosis, lymphoma, post-MI ECG: diffuse ST elevation and PR depression
internalmedicine rheumatology step2 -
Illustration: slide with highlighted teaching points — what image shows?
 Image: presentation slide with highlighted clinical teaching pointsinternalmedicine education step2
Image: presentation slide with highlighted clinical teaching pointsinternalmedicine education step2 -
Knee injury randomized trial with 500 randomized to operative (400 received) and 500 randomized to conventional (50 received): What is the primary study-design concern?
- Lack of intention-to-treat (ITT) analysis
surgery internalmedicine step2. -
Definition: What is intention-to-treat (ITT) analysis?
- Include all randomized subjects in the group originally assigned regardless of treatment actually received
internalmedicine surgery step2. -
Per-protocol analysis: how does it differ from ITT?
- Analyzes subjects according to the treatment actually received rather than original randomization
internalmedicine surgery step2. -
Why is lack of ITT analysis problematic in the knee trial described?
- Excluding randomized subjects introduces bias and reduces benefits of randomization, risking erroneous conclusions
surgery internalmedicine step2. -
When would 'Inadequate randomization' be the correct concern in a trial?
- When randomization method fails to account for or balance important factors/comorbidities that affect outcome
internalmedicine surgery step2. -
When is 'Inappropriate control group' (placebo) the correct concern?
- When an effective treatment exists or placebo use could cause harm; use standard-of-care control instead
internalmedicine surgery step2. -
When is 'Short follow-up duration' a valid trial concern?
- When short follow-up may miss late complications or fail to show durability of benefits; appropriateness depends on condition
internalmedicine surgery step2. -
Is 'Small sample size' the primary problem in the described knee trial?
- No. The trial enrolled 1000 patients, so small sample size is not the main concern
internalmedicine surgery step2. -
Study design: What is the effect of a 'small sample size' on statistical power?
- 'Small sample size' reduces statistical power, lowering ability to detect true differences between groups
internal step2. -
Clinical trial: Name baseline factors that influence statistical power (grouped).
- Baseline incidence of outcome
- Population variance
internal step2. -
Clinical trial: Name treatment-related factors that influence statistical power (grouped).
- Magnitude of treatment effect
- Likelihood of type I and type II errors
internal step2. -
Study planning: Is enrolling 1000 participants generally adequate for statistical power?
- Yes; in most instances enrollment of 1000 provides adequate statistical power
internal step2. -
Intention-to-treat (ITT): What is the ITT analysis rule for randomized subjects?
- Include all randomized subjects in analysis in the group to which they were originally randomized regardless of received treatment
internal step2. -
ITT rationale: What is the consequence of excluding randomized subjects from analysis?
- Excluding randomized subjects introduces bias and reduces prognostic benefit of randomization
internal step2. -
ITT benefit: What biases does ITT help limit and what integrity does it preserve?
- Preserves randomization integrity
- Limits attrition bias
internal step2. -
Intention-to-treat (ITT): Illustrative slide (supporting image on answer side).
- ITT = include all randomized by original group; preserves randomization and limits attrition bias
 internal step2.
internal step2. -
Anchor: Oncology unit medication errors — what root cause was identified?
- Look-alike medication packaging causing inadvertent antibiotic/chemotherapy swaps
internal_medicine step2. -
Anchor: Correct intervention to prevent look-alike vial errors in oncology unit?
- Repackage medications so containers are distinct (pharmacy-level packaging change)
internal_medicine step2. -
Anchor: Why is repackaging distinct containers the best fix for repeated look-alike medication errors?
- Targets systems-level cause identified by RCA; removes visual similarity that led to errors
internal_medicine step2. -
Anchor: Root cause analysis (RCA) — concise definition?
- Multidisciplinary process to define/analyze problems and design corrective actions based on analysis
internal_medicine step2. -
Anchor: Staff interviews — role in RCA?
- Staff interviews are a common RCA strategy to identify causes of adverse events
internal_medicine step2. -
Anchor: Option B ('Remove the antibiotic from formulary') — why is this incorrect here?
- Unnecessary and restricts effective antibiotic choices; repackaging suffices
internal_medicine step2. -
Anchor: Option C ('Require continuing education for nurses') — when would this be appropriate?
- Appropriate if errors result from knowledge/skill deficits rather than systems-level packaging similarity
internal_medicine step2. -
Anchor: Option D ('Suspend nurses involved') — why is suspension incorrect here?
- Blames individuals for system error; discourages reporting and hides problems
internal_medicine step2. -
Anchor: Option E ('No intervention likely helpful') — why is this incorrect here?
- RCA identified a modifiable cause (packaging); targeted repackaging is likely to prevent future errors
internal_medicine step2. -
Anchor: Common predictable cause of medication errors — what is it?
- Different medications appearing similar (look-alike packaging)
internal_medicine step2. -
Anchor: Example of a targeted corrective action for look-alike vials — what might be done by pharmacy?
- Repackage or relabel vials so appearance and containers are distinct
 internal_medicine step2.
internal_medicine step2. -
Squamous cell carcinoma of the lung: key paraneoplastic metabolic abnormality?
Hypercalcemia due to paraneoplastic parathyroid hormone-related peptide (PTHrP) production.
internal_medicine step2. -
Squamous cell carcinoma of the lung: typical gross/clinic location and radiographic feature?
Central location with pulmonary cavitations.
internal_medicine step2. -
Squamous cell carcinoma histology: characteristic findings?
- Polygonal cells with intercellular bridges
- Eosinophilic cytoplasm
- Keratin pearls
- Extensive necrosis
internal_medicine step2. -
internal_medicine step2.
-
internal_medicine step2.
-
Why squamous cell carcinoma is the correct diagnosis for a 3-cm central lung mass with hypercalcemia in a long-term smoker?
Smoking risk + central mass + hypercalcemia from PTHrP + squamous histologic features point to squamous cell carcinoma.
internal_medicine step2. -
Adenocarcinoma of the lung: typical patient profile and location?
More common in nonsmokers and females; peripheral lung location.
internal_medicine step2. -
internal_medicine step2.
-
Large cell carcinoma of the lung: defining histology and typical location?
Highly anaplastic, lacks glandular/squamous/neuroendocrine features; most often peripheral.
internal_medicine step2. -
Small cell carcinoma of the lung: cell type and distinguishing paraneoplastic syndromes?
- Neuroendocrine tumor of small dark blue cells
- Paraneoplastic: Cushing (ACTH), SIADH, Lambert-Eaton
internal_medicine step2. -
Small cell carcinoma histology distinctive microscopic appearance?
Small dark blue tumor cells with high nuclear-to-cytoplasm ratio and lacking nucleoli.
internal_medicine step2. -
Melanoma: typical primary lesion features and common metastatic sites?
- Primary: asymmetric, irregular borders, variable color, >6 mm, rapid change
- Metastases commonly to lung, brain, liver, skin
internal_medicine step2. -
Imaging/biopsy illustration for confirming lung cancer diagnosis (supplementary image)?
Diagnosis by chest x-ray and biopsy. Image:
 internal_medicine step2.
internal_medicine step2. -
Which primary lung cancers are typically centrally located?
- Squamous cell carcinoma of the lung
- Small cell carcinoma of the lung
internalmedicine step2 -
internalmedicine step2
-
What paraneoplastic syndrome is associated with squamous cell carcinoma of the lung?
- Hypercalcemia from parathyroid hormone-related peptide (PTHrP) production
internalmedicine step2 -
internalmedicine step2
-
internalmedicine step2
-
What is the typical timing of detection and its impact on prognosis for primary lung cancer?
- Often detected once metastatic → prognosis poor
internalmedicine step2 -
Diagnostic illustration for primary lung cancer (supplementary): what imaging and tissue test are used?
- Imaging: chest x-ray
- Tissue: biopsy
 internalmedicine step2
internalmedicine step2 -
Diagnosis: 62-year-old with 2 days nausea, severe abdominal pain, prior partial gastrectomy; CT shows target sign: what is the most likely diagnosis?
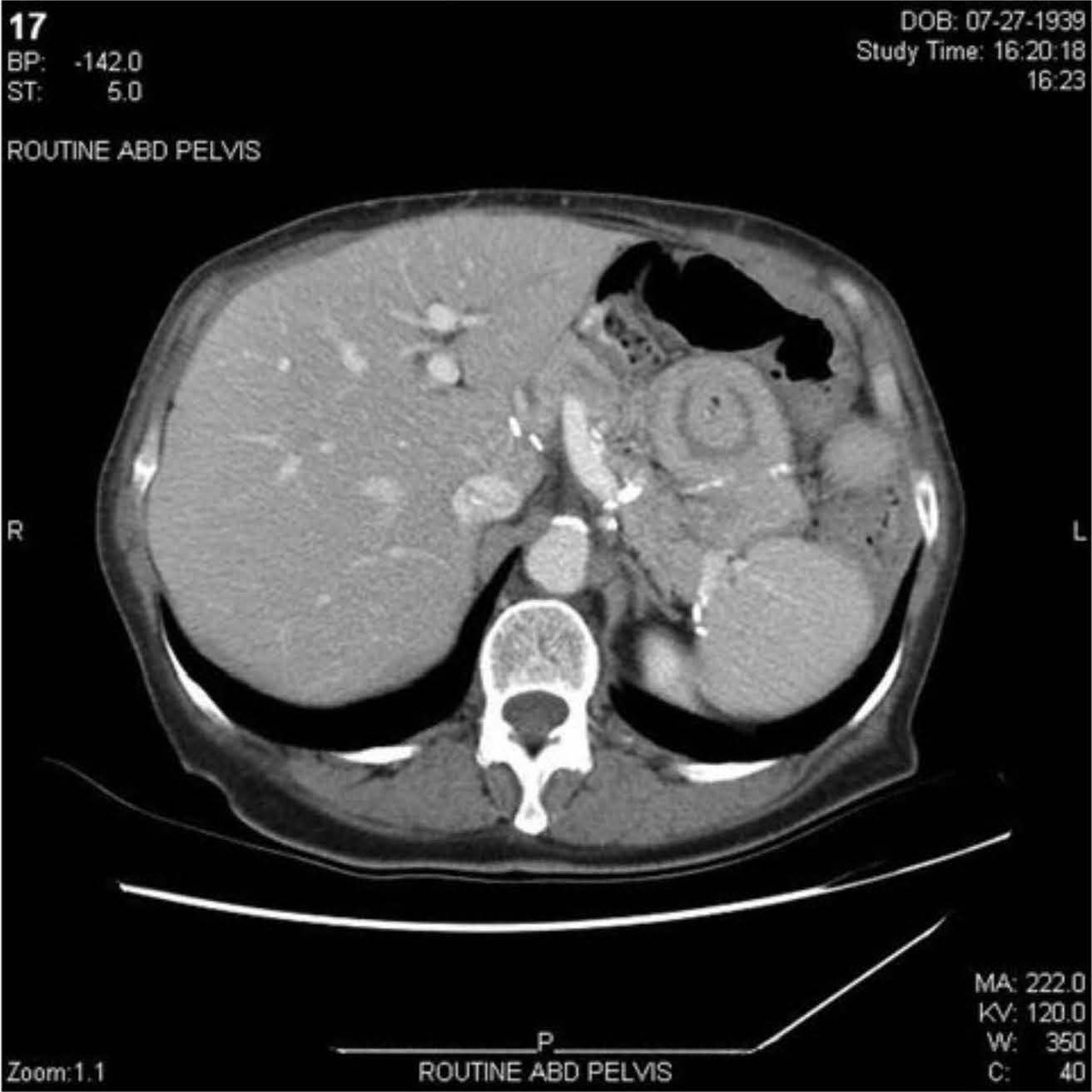
Intussusception
surgery internal_medicine step2. -
Pathophysiology: What causes intussusception? (anchor: intussusception)
Telescoping of one bowel segment into adjacent segment causing traction on mesenteric vessels → hypoperfusion, inflammation, hemorrhage, obstruction
surgery step2. -
Intussusception lead points: Name common pathologic lead points that precipitate intussusception.
- Lymphoid hyperplasia / lymphadenopathy
- Meckel diverticulum
- Adhesion, stricture, or malignancy
pediatrics surgery step2. -
Clinical features: What are typical symptoms of intussusception in adults? (anchor: intussusception symptoms)
- Colicky abdominal pain
- Nausea/vomiting
- Possible bloody mucoid stools
internal_medicine surgery step2. -
Imaging: What CT/US signs confirm intussusception? (anchor: intussusception imaging)
- Target sign on transverse imaging
- Telescoping bowel segments on longitudinal views
radiology surgery step2. -
Management: How does adult intussusception treatment differ from pediatric? (anchor: intussusception management)
- Adults: usually require surgical intervention
- Children: often treated with air or contrast enema
surgery pediatrics step2. -
When is bacterial small-bowel overgrowth the correct diagnosis? (anchor: bacterial overgrowth features)
Chronic impaired peristalsis → bacterial proliferation causing malabsorption, diarrhea, bloating, chronic pain; diagnosis via hydrogen breath test; responds to antibiotics
internal_medicine infectious_disease step2. -
When is intestinal volvulus the correct diagnosis? (anchor: volvulus features)
Twisting of bowel mesentery causing large-bowel obstruction; classic coffee-bean appearance on x-ray and marked bowel distension; risk of necrosis if untreated
surgery internal_medicine step2. -
When is jejunal enteritis the correct diagnosis? (anchor: jejunal enteritis features)
Mucosal infection/inflammation producing nausea, vomiting, cramping, diarrhea; may have fever or bloody stools; CT shows mucosal inflammatory changes but not target sign
infectious_disease internal_medicine step2. -
When are small-bowel adhesions the correct diagnosis? (anchor: small-bowel adhesions features)
History of prior intra-abdominal surgery → adhesions causing small-bowel obstruction (partial or complete) with bowel dilatation; most common SBO cause postop
surgery internal_medicine step2. -
Differentiation: How to distinguish intussusception from small-bowel adhesions on CT? (anchor: imaging differentiation)
- Intussusception: target sign, telescoping segments
- Adhesions: SBO pattern with transition point and dilated proximal bowel but no target sign
radiology surgery step2. -
Clinical context: Why could prior partial gastrectomy predispose an adult to intussusception? (anchor: postop risk)
Prior abdominal surgery can create lead points (adhesions/structural changes) that trigger bowel telescoping during peristalsis
surgery internal_medicine step2. -
surgery internalmedicine step2.
-
surgery radiology step2.
-
Why does absence of dilated small bowel loops on CT argue against SBO?
- Lack of dilated loops + air-fluid levels makes classic SBO imaging absent, reducing likelihood of SBO
surgery internalmedicine step2. -
surgery internalmedicine step2.
-
surgery internalmedicine step2.
-
Intussusception: pathophysiology (anchor: Intussusception)?
- One bowel segment telescopes into adjacent segment
pediatrics surgery step2. -
Intussusception: classic clinical features?
- Colicky abdominal pain, nausea/vomiting, possible bloody mucoid stools
pediatrics internalmedicine step2. -
Imaging signs of intussusception on CT or ultrasound?
- Longitudinal: telescoping bowel segments
- Transverse: 'target sign'
radiology pediatrics step2. -
Clinical decision: When would exploratory laparotomy be indicated for bowel obstruction?
- Complete obstruction or complicated partial obstruction
surgery internalmedicine step2. -
Interpretation task: Does this CT image support SBO? (anchor: CT abdomen)
Review for dilated small bowel loops and multiple air-fluid levels; absence of these findings argues against SBO
radiology surgery step2. -
CT example (anchor: CT abdomen image): view the image for landmarks relevant to obstruction.
 - Use image to assess loop dilation and air-fluid levelsradiology surgery step2.
- Use image to assess loop dilation and air-fluid levelsradiology surgery step2. -
Anaphylaxis: core pathophysiology?
- IgE-mediated mast cell/basophil activation → histamine and cytokine release → acute inflammation and widespread vasodilation
pediatrics step2. -
internal_medicine step2.
-
Anaphylaxis: organ systems commonly affected?
- Cardiovascular
- Respiratory
- Gastrointestinal
- Integumentary
emergency step2. -
Anaphylaxis: key presenting symptoms from each system (short)?
- Respiratory: bronchospasm, dyspnea, wheeze, stridor
- Skin: urticaria, flushing
- Cardiovascular: hypotension, tachycardia
- GI: nausea, vomiting
pediatrics step2. -
Stridor in anaphylaxis: clinical significance?
Stridor indicates glottic/subglottic angioedema and warns of impending airway loss
surgery step2. -
Initial management of anaphylaxis with hypotension, urticaria, stridor?
Urgent administration of epinephrine first
emergency step2. -
Why is epinephrine the first treatment in anaphylaxis?
Epinephrine causes vasoconstriction and reduces airway edema, reversing hypotension and airway obstruction
internal_medicine step2. -
Role of antihistamines in anaphylaxis?
Antihistamines are adjunctive therapy but should follow epinephrine
internal_medicine step2. -
Role of IV fluids in anaphylaxis?
IV fluids support intravascular volume for perfusion but follow epinephrine
internal_medicine step2. -
When is endotracheal intubation indicated in anaphylaxis?
If stridor or airway edema persists or worsens despite epinephrine, perform urgent intubation by most experienced provider
anesthesia step2. -
Risks/considerations for intubation in anaphylaxis?
Upper airway edema makes intubation difficult; may require surgical airway if intubation fails
surgery step2. -
Correct answer justification: why 'administration of epinephrine' is preferred over hospital admission alone?
Admission alone delays urgent reversal of vasodilation and airway edema; epinephrine must be given immediately to prevent shock and airway obstruction
pediatrics step2. -
When would antihistamine alone be appropriate for allergic reaction?
Antihistamine alone is only for mild, non-anaphylactic urticaria without respiratory or cardiovascular compromise
internal_medicine step2. -
Use of the provided image as illustration for airway edema?
Image: presentation slide (illustration only)
 emergency step2.
emergency step2. -
What is the pathophysiology of anaphylaxis?
Mast cell and basophil degranulation → acute multisystem inflammation and vasodilation
internal_medicine step2. -
pediatrics step2.
-
What are the main cutaneous/oral features of anaphylaxis?
- Urticaria
- Flushing
- Edematous lips and tongue
allergy step2. -
What are the main gastrointestinal and hemodynamic features of anaphylaxis?
- Nausea and emesis
- Hypotension with tachycardia
emergency step2. -
internal_medicine step2.
-
What are the next immediate adjunct treatments after epinephrine in anaphylaxis (group 1)?
- Antihistamines
- Bronchodilators
- Glucocorticoids
internal_medicine step2. -
What supportive measure is given after epinephrine and adjunct medications in anaphylaxis (group 2)?
- Fluids (intravenous) for hypotension
critical_care step2. -
Describe a concise treatment sequence for anaphylaxis.
- Epinephrine (urgent)
- Antihistamines, bronchodilators, glucocorticoids
- IV fluids
 emergency step2.
emergency step2. -
Diagnosis: Which eating disorder fits a 24-year-old with weekly binge eating and daily laxative purging, BMI 21, no vomiting?
- Bulimia nervosa (binge-eating with purging)
psychiatry step2. -
Pathophysiology: How does chronic laxative overuse cause metabolic acidosis?
- Loss of bicarbonate in stool → non-anion gap metabolic acidosis
internalmedicine step2. -
Pathophysiology: Mechanisms producing hypokalemia with chronic laxative abuse?
- Direct K+ loss in stool
- Hypovolemia → ↑aldosterone → renal K+ secretion
nephrology step2. -
Clinical feature: What orthostatic vital sign changes indicate hypovolemia in this patient?
- Supine 80/min → standing 90/min; BP supine 120/80 → standing 80/55; light-headedness on standing
internalmedicine step2. -
Diagnostics: Which laboratory pattern matches laxative-induced metabolic acidosis with hypokalemia (correct answer choice)?
- Serum K+ 3 mEq/L; ABG: pH 7.3, PCO2 30 mm Hg, HCO3- 14 mEq/L, PO2 90 mm Hg
internalmedicine step2. -
Why choice A would be correct: When does hyperkalemia with metabolic acidosis and respiratory compensation occur?
- Renal failure or acute acid load causing decreased K+ excretion → hyperkalemia + metabolic acidosis with respiratory compensation
nephrology step2. -
Why choice B would be correct: When does hypokalemia with metabolic alkalosis occur?
- Prolonged vomiting or diuretic use → loss of H+ and volume → metabolic alkalosis with hypokalemia via aldosterone
internalmedicine step2. -
Why choice D is incorrect: What does normal serum K+ and normal pH indicate?
- Normal electrolyte/acid-base status; not consistent with chronic laxative-induced stool losses causing pH/K+ abnormalities
internalmedicine step2. -
Why choice E would be correct: When is respiratory alkalosis with near-normal K+ seen?
- Hyperventilation (eg, anxiety, pain) → low PCO2 → respiratory alkalosis; K+ often near normal
pulmonology step2. -
Management: Immediate treatment priorities for bulimia nervosa with laxative-induced hypovolemia/hypokalemia?
- Correct volume depletion and electrolytes
- Start combined medical + psychiatric therapy (behavioral + pharmacologic)
psychiatry internalmedicine step2. -
Diagnostic distinction: How to differentiate laxative-induced acid-base disorder from vomiting-induced disorder?
- Laxatives → non-anion gap metabolic acidosis (low HCO3-)
- Vomiting → metabolic alkalosis (high HCO3-)
internalmedicine step2. -
Supplementary: Slide illustrating teaching points about laxative abuse and labs (image on answer side).
- Illustration:

- Content: laxative overuse → HCO3- loss, hypokalemia, hypovolemia signs, treat fluids/electrolytes + psychiatric care
psychiatry step2. - Illustration:
-
Disease: Bulimia nervosa — core behavioral features?
- Recurrent uncontrolled binge eating
- Compensatory purging (vomiting, laxatives, diuretics)
psychiatry step2 -
internal step2
-
Anchor: Laxative overuse — typical acid–base disturbance?
Metabolic acidosis due to stool bicarbonate loss
internal step2 -
Anchor: Laxative-induced hypokalemia — link to acid–base status?
Potassium wasting in stool occurs together with bicarbonate loss → hypokalemia + metabolic acidosis
internal step2 -
Anchor: Laxative overuse — effect on respiration?
Does NOT directly alter respiration; causes metabolic pH derangements instead
internal step2 -
internal psychiatry step2
-
Anchor: Vomiting vs laxative overuse — distinguishing acid–base effects?
- Vomiting → metabolic alkalosis (loss of acid)
- Laxatives → metabolic acidosis (loss of bicarbonate)
internal step2 -
Anchor: Compensatory purging options in bulimia (three main)?
- Self-induced vomiting
- Laxative overuse
- Diuretic overuse
psychiatry step2 -
Anchor: Image — visual slide of highlighted teaching point (supplement)
 Slide illustrates the teaching that laxative overuse causes K+ and HCO3− loss leading to hypokalemic metabolic acidosisinternal step2
Slide illustrates the teaching that laxative overuse causes K+ and HCO3− loss leading to hypokalemic metabolic acidosisinternal step2 -
Gentamicin: primary nephrotoxicity prevention measure when given IV for sepsis/UTI?
- Measure plasma aminoglycoside trough concentrations to avoid supratherapeutic levels and reduce nephrotoxicity
internalmedicine renal infectious step2. -
Gentamicin: mechanism of synergy with beta-lactams (eg, piperacillin-tazobactam)?
- Aminoglycosides + penicillins produce stronger combined bactericidal effect (synergy)
infectious internalmedicine step2. -
Gentamicin: major toxicities relevant to a 67-year-old with sepsis?
- Ototoxicity, nephrotoxicity, neurotoxicity
renal internalmedicine step2. -
Trough concentration: timing and meaning for aminoglycoside dosing?
- Trough = serum level immediately before next dose; reflects nadir after tissue redistribution and metabolism
pharmacology internalmedicine step2. -
Initial management of septic UTI with hypotension and CVA tenderness?
- IV fluids + broad-spectrum antibiotics (eg, piperacillin-tazobactam + gentamicin) immediately
internalmedicine infectious step2. -
Central venous pressure (CVP) measurement: when is it used clinically?
- Estimate right atrial pressure/preload; used to assess volume status in shock
surgery internalmedicine step2. -
CVP measurement: when would CVP likely be decreased?
- Distributive shock (eg, septic shock) causes decreased CVP due to vasodilation and low preload
internalmedicine criticalcare step2. -
Piperacillin-tazobactam: role in urosepsis and nephrotoxicity risk?
- Covers gram-negative rods and anaerobes; needed for urosepsis; generally less nephrotoxic than gentamicin
infectious internalmedicine step2. -
When is discontinuation of piperacillin-tazobactam appropriate in sepsis?
- Only if alternative narrower therapy available or allergic/toxic effect identified; not initial step in urosepsis
infectious internalmedicine step2. -
Bicarbonate therapy: appropriate indication in septic patient?
- Severe metabolic acidosis; not indicated without diagnosed metabolic acidosis
internalmedicine criticalcare step2. -
Low-dose dopamine: typical clinical use compared with norepinephrine?
- Used for cardiogenic shock/advanced heart failure; norepinephrine preferred initial vasopressor for septic shock
cardiology internalmedicine step2. -
Why measuring gentamicin trough is correct choice to reduce acute renal failure risk?
- Trough monitoring prevents supratherapeutic gentamicin levels, lowering nephrotoxicity risk during IV aminoglycoside therapy
renal pharmacology step2. -
Image: Urosepsis with right CVA tenderness — which supportive therapy is essential before vasopressors?
- IV fluids are immediate therapy for hypotension in septic UTI; image for illustration:
internalmedicine infectious step2. - IV fluids are immediate therapy for hypotension in septic UTI; image for illustration:
-
internalmedicine pharmacology step2. pediatrics
-
Gentamicin: clinical purpose of measuring trough concentration?
- Predict and help prevent nephrotoxicity
 internalmedicine pharmacology step2. pediatrics
internalmedicine pharmacology step2. pediatrics -
Screening: Which preventive test is most appropriate now for a 47-year-old obese woman (BMI 33) to detect type 2 diabetes?
Measure fasting serum glucose or hemoglobin A1c now
internalmedicine obgyn step2. -
Rationale: Why screen for diabetes in adults aged 35–70 who are overweight/obese?
Overweight/obese adults 35–70 have recommended fasting glucose or A1c testing to detect type 2 diabetes early and reduce morbidity/mortality
internalmedicine step2. -
Pap smear: When is cervical cancer screening recommended for a 47-year-old woman with prior normal Pap smears?
Pap smear every 3 years or every 5 years with normal HPV cotesting; annual Pap not indicated
obgyn step2. -
DEXA scan: When is osteoporosis screening indicated instead of now for this 47-year-old premenopausal woman?
DEXA screening recommended ≥65 years or postmenopausal with major risk factors (eg, low weight, chronic glucocorticoids); not routine premenopausal
internalmedicine obgyn step2. -
ECG screening: When is a resting ECG the most appropriate screening test in asymptomatic adults like this patient?
Routine ECG not indicated for asymptomatic low-risk adults; use when symptoms or specific cardiovascular concerns exist
cardiology internalmedicine step2. -
Mammography: What is the recommended screening interval relevant to a 47-year-old woman?
Begin breast cancer screening between ages 40–50; intervals vary by guideline (eg, annually or biennially); mammography every 3 years is not standard
obgyn internalmedicine step2. -
Comparison: Why is fasting glucose/A1c preferred now over Pap smear, DEXA, ECG, or mammography for this patient?
Patient is 47 and obese (BMI 33): diabetes screening age/risk criteria met; other tests either not due (Pap), not indicated (DEXA premenopausal), unnecessary routinely (ECG), or interval/guideline-dependent (mammography)
internalmedicine obgyn step2. -
Guidelines summary: Which two screening categories encompass most adult preventive recommendations mentioned?
Cardiovascular risk assessment and cancer screening
internalmedicine step2. -
Illustration: Where to find recommended screening example for overweight 35–70-year-olds (image)?
Guideline slide showing diabetes screening recommendation:
 internalmedicine step2.
internalmedicine step2. -
Baseline ECG screening: When is an ECG indicated?
- When cardiovascular symptoms are present (eg, exertional chest pain, dyspnea, palpitations)
- When electrolyte disturbance or medication side effects suspected
- To evaluate resting angina
internal step2. -
Baseline ECG screening in asymptomatic adults: why is it not recommended?
- Inconsistent abnormal findings in asymptomatic people and can be normal in existing disease
- Leads to unnecessary testing and potential harm
internal step2. -
When is screening mammography routinely recommended by USPSTF?
- Every 1–2 years for patients >50 years
obgyn step2. -
Breast cancer screening for patients aged 40–49 years: what is the recommendation?
- Shared decision-making between patient and physician; decision depends on balance of benefits vs risks
obgyn step2. -
Why is mammography every 3 years incorrect for a 47-year-old patient?
- 47-year-old falls in 40–49 group where screening is a shared decision; USPSTF recommends 1–2 years for >50, not routine 3-year interval
obgyn step2. -
Screening for type 2 diabetes mellitus: which patients should be screened?
- Overweight or obese patients aged 35–70 years using fasting glucose or hemoglobin A1c
internal step2. -
Preventive care screening decisions: what factors determine recommendations?
- Patient sex, age, and other risk factors determine screening recommendations
internal step2. -
Illustration: Which screening topic is highlighted in the slide?
- Slide illustrates preventive-screening recommendations (eg, ECG, mammography, diabetes screening)
 internal step2.
internal step2. -
Restless legs syndrome (RLS): core diagnostic features?
- Unpleasant leg sensations at rest or during sleep
- Partial relief with movement
- Causes distress or functional impairment
neurology internal_medicine step2 -
RLS: common associated pathophysiology mentioned?
- Abnormal dopaminergic signaling
- Abnormal iron homeostasis
neurology internal_medicine step2 -
Role of serum ferritin in RLS diagnosis?
Decreased serum ferritin is associated with RLS exacerbation and helps confirm diagnosis
internal_medicine neurology step2 -
Iron supplementation in RLS: when recommended?
- Give iron supplementation for symptom improvement in patients with or without low ferritin
internal_medicine neurology step2 -
First-line treatments for RLS?
- Sleep-hygiene and lifestyle measures
- Iron supplementation
- Dopaminergic agonists (eg, ropinirole)
neurology internal_medicine step2 -
Why measurement of serum ferritin was the most appropriate next diagnostic step in this 47-year-old with bilateral leg restlessness?
Ferritin assesses iron stores; low ferritin associates with RLS and guides diagnosis/iron therapy
internal_medicine neurology step2 -
When is Doppler ultrasonography of lower extremities appropriate (vs RLS)?
Use Doppler to evaluate suspected DVT or PAD presenting with unilateral leg pain/swelling or exertional limb pain, not bilateral rest-related restlessness
surgery internal_medicine step2 -
When is EEG appropriate for nocturnal symptoms (vs RLS)?
EEG helps diagnose seizures or sleep arousals from epilepsy; not required when presentation fits RLS without seizure features
neurology psychiatry step2 -
When is fasting serum glucose useful for leg symptoms (vs RLS)?
Check fasting glucose to evaluate diabetes when suspected diabetic neuropathy causing sensory/motor deficits in a stocking‑glove distribution
internal_medicine endocrinology step2 -
Why 'no further testing' is incorrect for this patient?
Testing ferritin can confirm RLS and guide iron therapy; therefore at least ferritin measurement is indicated
internal_medicine neurology step2 -
Distinguishing feature: RLS vs peripheral arterial disease (PAD)?
RLS symptoms occur at rest and improve with movement; PAD causes activity‑provoked claudication relieved by rest
internal_medicine vascular_surgery step2 -
Distinguishing feature: RLS vs deep vein thrombosis (DVT)?
DVT usually causes unilateral leg pain and swelling; RLS causes bilateral rest-related unpleasant sensations without overt swelling
surgery internal_medicine step2 -
Distinguishing feature: RLS vs diabetic peripheral neuropathy?
Diabetic neuropathy causes sensory loss and weakness in stocking‑glove distribution; RLS has normal strength and light-touch sensation with rest‑provoked discomfort
internal_medicine neurology step2 -
Use of provided image as supplementary material for RLS education
 Image illustrates teaching points; do not use to identify diagnosisneurology internal_medicine step2
Image illustrates teaching points; do not use to identify diagnosisneurology internal_medicine step2 -
Scaphoid fracture: typical mechanism and common location
- Fall onto outstretched hand
- Scaphoid is most commonly fractured carpal bone
surgery step2. -
Scaphoid fracture: presenting exam findings
- Wrist pain with swelling
- Tenderness in anatomical snuffbox (between extensor pollicis longus and brevis)
internal_medicine step2. -
Scaphoid blood supply relevance to complications
Blood supply enters distally from a branch of the radial artery, placing proximal pole fractures at risk for nonunion and necrosis
surgery step2. -
orthopedics step2.
-
Initial imaging and next step if x-ray unremarkable but suspicion remains
- X-ray initial imaging
- If x-ray unremarkable and high suspicion: immobilize and repeat x-rays in 2–3 weeks
radiology step2. -
surgery step2.
-
Displaced scaphoid fracture: management consideration
Surgery may be indicated for displaced fractures
surgery step2. -
When is distal fat embolus expected after orthopedic trauma?
After pelvic or long-bone fractures due to bone marrow fat entering bloodstream; causes respiratory, neurologic, or petechial findings
critical step2. -
Osteomyelitis: diagnostic features distinguishing it from simple fracture
Infection with ↑ inflammatory markers (ESR, CRP) and radiographic lytic lesions or cortical destruction
infectious step2. -
Malunion of scaphoid fracture: expected consequence
Poor angulation causing pain or altered wrist biomechanics after healing
surgery step2. -
Wrist fusion in scaphoid disease: when considered
Considered after noninvasive measures fail for pain from nonunion or necrosis
orthopedics step2. -
Use of the provided image for scaphoid fracture learning
Image shows highlighted teaching slide; use as illustration for scaphoid fracture features and management
 education step2.
education step2. -
surgery step2.
-
Scaphoid blood supply and clinical consequence?
- Distal blood supply from a radial artery branch → risk of nonunion
surgery step2. -
surgery step2.
-
Scaphoid fracture: indications for surgical intervention?
- Displaced fractures
- Proximal pole fractures
surgery step2. -
Scaphoid fracture: why proximal pole fractures favor surgery?
- Proximal pole has poorer blood supply → higher nonunion risk → surgery recommended
 surgery step2.
surgery step2.
High-yield clinical notes (NBME-style cases)
Ethics & decision-making
- Assess decisional capacity first (case: 90-year-old refusing surgery). Capacity is decision-specific and requires the patient to: 1) express a consistent choice, 2) understand risks/benefits, 3) appreciate personal consequences, and 4) reason about options. If capacity intact, respect autonomy; if not, use durable power of attorney/ surrogate. Competence is a legal determination.
General diagnostic principles
- Single abnormal vital sign or lab rarely proves chronic disease (eg, one high BP does NOT equal hypertension). Confirm with repeat or home/serial measurements before workup for secondary causes.
- Use targeted tests: reserve complex imaging/ invasive tests for when they will change management (eg, CT angio for suspected PE when pretest probability high).
Trauma / Emergency
- Hemothorax after blunt chest trauma: immediate management = tube thoracostomy to drain blood, re-expand lung, and monitor ongoing bleeding (massive hemothorax if >1000–1500 mL initial or >200 mL/hr × 4 h).
- Intubation / airway: in anaphylaxis with stridor, give epinephrine immediately; if airway fails to improve or obstruction worsens, prepare for urgent intubation or surgical airway.
Pulmonary conditions
- Pulmonary embolism (PE): suspect with sudden dyspnea/hypoxemia and risk factors (immobility, obesity, recent surgery); spiral CT chest (CT pulmonary angiography) is preferred confirmatory test when clinical suspicion is high.
- Cardiogenic shock after MI: first-line inotropic support = dobutamine (B1 agonist) to increase contractility; vasopressors (eg, norepinephrine) may be used adjunctively if needed.
- Bacterial tracheitis (child with high fever, inspiratory stridor, no response to racemic epinephrine): think bacterial tracheitis — treat with antibiotics + steroids; airway surveillance (may need intubation).
Infectious diseases & prophylaxis
- Meningococcal exposure: give chemoprophylaxis to close contacts (rifampin, ciprofloxacin, or ceftriaxone), not all ED personnel.
- Postpartum endometritis: fever, foul lochia, uterine fundal tenderness after C-section → start broad-spectrum antibiotics promptly (eg, clindamycin + gentamicin) rather than routine imaging.
- Splenectomy preop vaccines: vaccinate against encapsulated organisms: Streptococcus pneumoniae, Haemophilus influenzae type b, Neisseria meningitidis (give before splenectomy if possible).
Cardiac / vascular
- Right ventricular infarction (inferior MI with V4R–V6R changes): patients often are preload-dependent — give IV crystalloids (saline) as initial stabilization rather than diuretics or negative inotropes.
- Amaurosis fugax / Hollenhorst plaque: visible yellow refractile plaque in retinal arterioles suggests cholesterol embolus; evaluate with carotid duplex (ipsilateral carotid is common source).
- Atrial septal defect (fixed wide split S2) → chronic left-to-right shunt → risk of pulmonary vascular remodeling and later pulmonary hypertension/Eisenmenger if uncorrected.
Renal / GU
- Single functional kidney with hydronephrosis/obstruction: if imaging shows proximal obstruction and worsening renal function, percutaneous nephrostomy to decompress is appropriate as a temporizing measure.
- Gentamicin/aminoglycoside use in sepsis: monitor trough (and peak) levels to reduce nephrotoxicity risk; adjust dosing based on troughs.
- Septic shock with refractory hypotension: consider IV hydrocortisone for possible relative adrenal insufficiency when fluids + vasopressors inadequate and electrolytes suggest adrenal dysfunction.
Nephrology / transplant
- Tertiary hyperparathyroidism (long-standing CKD/transplant): persistent high PTH with hypercalcemia due to parathyroid hyperplasia and autonomous secretion; treat surgical parathyroidectomy if refractory.
- Membranous nephropathy (nephrotic): ACE inhibitors (eg, lisinopril) reduce intraglomerular pressure (efferent dilation) and slow progression by reducing hyperfiltration injury.
Hematology / transfusion
- Isoimmunization to RBC antigens (eg, Kell): strongest risk factor = prior blood transfusion (greater blood exposure increases alloimmunization risk) — important in pregnancy counseling and paternal antigen testing.
Gastroenterology / hepatology
- Acute viral hepatitis: very high AST/ALT (often >1000 U/L), +/- modest leukocytosis; supportive care while identifying specific viral cause.
- Pancreatic cancer suspicion: painless jaundice, weight loss, epigastric fullness, cholestatic labs → CT abdomen with contrast is the initial imaging of choice to evaluate for pancreatic mass.
GI/abdominal emergencies in adults
- Intussusception in adults: less common than in children, usually pathologic lead point; CT abdomen may show the "target sign" (telescoping bowel) — adult cases usually need surgical management.
Musculoskeletal / ortho
- Scaphoid fracture (fall on outstretched hand): common carpal fracture; frequent complication = nonunion due to retrograde/limited blood supply to proximal pole — immobilize and follow-up imaging; consider surgery if displaced.
- Spinal degenerative disease / chronic low back pain: in absence of red flags or focal neuro deficits, plain lumbar x-rays are an appropriate initial imaging test; reserve MRI for neurologic deficits or surgical planning.
Pediatrics
- Osteomyelitis (hematogenous, child): fever, refusal to bear weight, marrow edema on MRI; blood cultures and Gram stain guide therapy — vancomycin empirically for suspected MRSA in children until sensitivities return.
- Child with anaphylaxis while eating: immediate IM/IV epinephrine is first-line therapy.
- Bacterial tracheitis vs croup: unresponsive stridor and high fever after epinephrine suggests bacterial tracheitis — treat with antibiotics and airway monitoring.
Obstetrics / gynecology
- Rho(D) and other RBC antibodies: prior blood transfusion is a major risk for isoimmunization (eg, anti-Kell). Determine paternal antigen status to assess fetal risk; close monitoring or intervention if fetus at risk.
- Post-splenectomy: ensure vaccines against encapsulated organisms prior to surgery when possible.
Dermatology
- Cherry angiomas: common benign vascular papules appearing after age ~30; no workup needed and removal optional for cosmesis.
 Alt: Cherry angiomas on skin, multiple small red papules.
Alt: Cherry angiomas on skin, multiple small red papules.
Ophthalmology
- Hollenhorst plaque (cholesterol embolus) → transient monocular vision loss (amaurosis fugax); next step = carotid duplex to look for ipsilateral carotid atherosclerosis.
 Alt: Fundus photo with bright refractile plaque in a retinal arteriole.
Alt: Fundus photo with bright refractile plaque in a retinal arteriole.
Dermatology / EENT quick points
- Bacterial vaginosis: gray malodorous discharge + clue cells on wet mount; treat with metronidazole.
- Cherry angiomas: benign, no testing required.
Endocrine / metabolic
- Bulimia with chronic laxative abuse: expect hypokalemia and non–anion-gap metabolic acidosis (loss of bicarbonate in stool); orthostatic hypotension from volume depletion is common.
- Restless legs syndrome (RLS): assess serum ferritin (iron deficiency worsens RLS); treat with iron repletion and dopamine agonists if symptomatic.
Oncology / pathology
- Lung cancer histology clues: central mass + hypercalcemia → squamous cell carcinoma (keratinization, intercellular bridges). Peripheral masses and nonsmokers → adenocarcinoma.
- Hodgkin lymphoma: Reed-Sternberg cells on node biopsy → next step = staging imaging (CT or PET) to assess distribution and plan therapy.
Pharmacology & toxicology
- Aminoglycosides (eg, gentamicin): nephrotoxicity risk — monitor trough levels and adjust dosing to prevent AKI.
- Hypertensive emergency due to sympathomimetics (eg, phentermine): use an α-blocker (eg, phentolamine) or direct vasodilator (eg, sodium nitroprusside); avoid β-blockers alone if α stimulation present.
Quality improvement & study design
- Medication errors from look-alike packaging: root-cause analysis often leads to systems fix (eg, repackage/relabel vials) rather than blaming staff.
- Intention-to-treat (ITT) analysis vs per-protocol: ITT preserves randomization and avoids bias; analyzing subjects by treatment actually received can produce misleading results.
- Statistical vs clinical significance: a small absolute difference can be statistically significant (P<0.05) but lack clinical relevance; consider absolute risk reduction and number needed to treat.
Imaging examples (selected)
- Chest x-ray (PE suspicion): may be nonspecific; if high suspicion, proceed to CT pulmonary angiography.
 Alt: Chest x-ray used in PE case.
Alt: Chest x-ray used in PE case.
- CT abdomen with target sign: adult intussusception can show telescoped bowel with concentric rings/target appearance — usually surgical management.
 Alt: CT abdomen with target sign consistent with intussusception.
Alt: CT abdomen with target sign consistent with intussusception.
Study tips: focus on pattern recognition (presenting features → likely diagnosis) and the single most important immediate management step for emergencies (eg, epinephrine for anaphylaxis; chest tube for hemothorax; CT angio for PE; dobutamine for cardiogenic shock).