Sign up to unlock more features
- Save this deck to your account
- Study flashcards with spaced repetition
- Export to Anki (.apkg) or PDF
- Process documents up to 100 pages
- Images extracted from PDFs and documents
- Better text extraction from your PDFs and documents
- Better flashcards with our more advanced AI model
Flashcards in this deck (48)
-
What is the primary role of platelets in the vasculature?
- Circulate as quiescent cells and survey vascular integrity
- Undergo explosive activation upon vessel wall damage
-
How are platelets described metaphorically in the lecture?
They are described as the 'unmanned drones of the vasculature'
-
What is the cellular origin and nuclear status of platelets?
- Anucleate discs derived from megakaryocyte
-
-
-
What is the normal platelet count range provided in the notes?
Normal platelet count: 150 - 400 x 10 /litre
-
Name the main ultrastructural components shown in the platelet diagram.
- Glycogen
- Phospholipid membrane
- Open canalicular system
- Mitochondrion
- Dense granules
- Alpha granules
-
List the platelet surface receptors provided in the text.
- Gp VI
- Gp Ib-IX-V complex
- Gp IIb-IIIa complex
-
Which substances are contained in platelet dense granules according to the text?
- Ca
- ADP / ATP
- Serotonin
-
Which substances are listed as contents of the (alpha) granules in the text?
- VWF
- Fibrinogen
- Factor V
- PF4
-
-
Which binding sites does VWF contain?
- Binding sites for platelets
- Binding sites for sub-endothelial tissue
-
What is required for VWF binding sites to become exposed?
- VWF must be 'tethered' for its binding sites to be exposed

-
-
How is the GPIb‑V‑IX complex connected within the platelet?
- It is coupled to the underlying cytoskeleton.
-
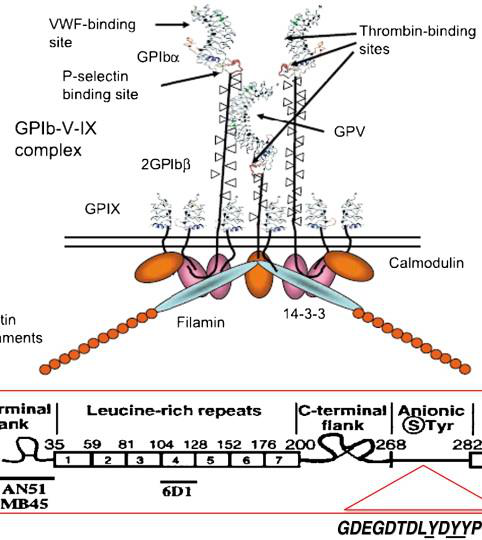
Which molecular interactions are shown for the GPIb‑V‑IX complex in the schematic?
- Interactions with VWF, P‑selectin, Thrombin, Filamin, and Calmodulin
-
What is the VWF-GPIba complex?
- Interaction between a circulating plasma protein (Von Willebrand Factor; VWF) and a platelet surface receptor (glycoprotein Ib; GPIba).
-
What is the primary function of the VWF-GPIba complex?
- It is crucial for platelet adhesion in high shear conditions.
-
What are the sequential steps by which von Willebrand factor (VWF) mediates platelet adhesion at a vascular injury site?
- VWF becomes tethered to the site of vascular injury
- VWF unravels, exposing binding sites for GPIbα
- Platelets bind to the site of injury via GPIb

-
Which change in VWF exposes platelet-binding sites for GPIbα?
VWF unravels, which exposes binding sites for GPIbα.
-
What is Von Willebrand disease (VWD) and how common is it?
- Von Willebrand disease (VWD): the most common bleeding disorder
- Prevalence: ~1 in 1000
-
What general cause underlies Von Willebrand disease according to the text?
- Cause: Genetic defects in von Willebrand factor (VWF)
-
List the specific functional consequences of VWF genetic defects described in the text.
- Consequences:
- Low VWF levels
- Inability of VWF to bind collagen or platelets
- Failure to bind sub-endothelial tissue or platelets
-
What is Bernard-Soulier syndrome?
- Bernard-Soulier syndrome is a rare genetic defect in GPIba that prevents normal von Willebrand factor (VWF) interaction.
-
How does the GPIba defect in Bernard-Soulier syndrome affect platelet function?
- The GPIba defect prevents normal VWF–GPIb interaction, which prevents normal thrombus formation.
-
What is the primary clinical consequence of Bernard-Soulier syndrome?
- A bleeding tendency due to impaired thrombus formation.
-
What are the main steps of platelet activation?
- Change in platelet shape
- Activation of cell surface integrins (Gpllb/llla)
- Granule secretion
- 'Flip/Flop' of plasma membrane
-
-
What are the purposes of platelet 'activation' in haemostasis?
- Adopt structural changes to help clot formation
- Secretion of factors that facilitate clot formation
- Activate cell surface molecules to make them 'sticky' for other platelets and coagulation factors
-
-
-
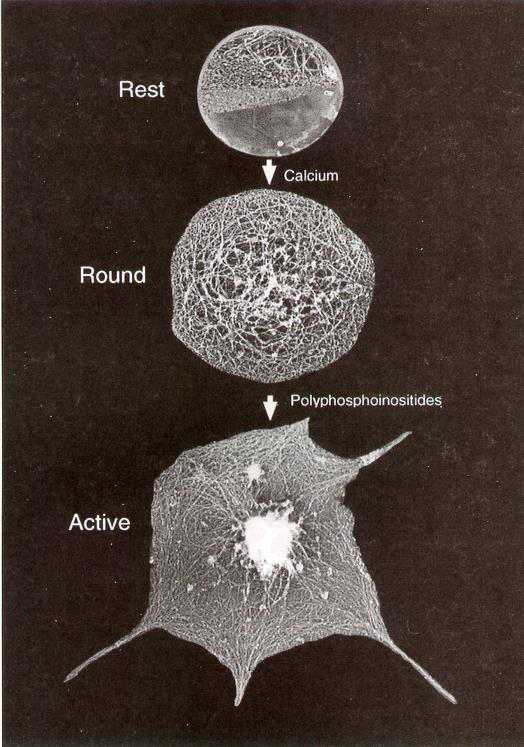
What cytoskeletal change underlies platelet shape change?
Reorder of actin and tubulin polymers of the cytoskeleton
Answer image:
-
What are the main platelet granule types and their primary contents/functions?
- Dense granules: rich in chemical messengers that promote further platelet activation and aggregation
- Alpha granules: rich in clotting proteins and contribute to further clot formation
-
What is the open canalicular system (OCS) in platelets?
An extensive system of internal membrane tunnels that serves as a conduit system for granule release.
-
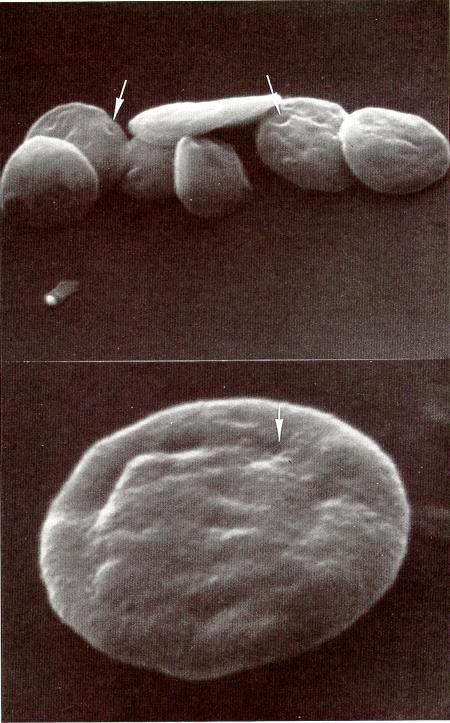
What structural feature on the platelet surface forms the entrances into the OCS?
- Periodic invaginations on a flat platelet surface
-
What is the primary clinical use of inhibitors of platelet activation?
- To prevent arterial thrombosis (lesions rich in aggregated platelets)
-
-
By what mechanism do inhibitors of platelet activation act?
- They inhibit signaling pathways that lead to platelet activation
-
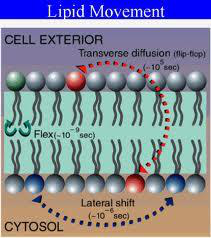
What does 'flip-flop' of phospholipids refer to in platelet membranes?
The transverse movement where negatively charged phospholipids that were on the inner leaflet become externalized to the outer leaflet of the platelet membrane.
-
Why is phospholipid externalization on activated platelets important for coagulation?
- It is necessary for vitamin K-dependent coagulation factor binding
-
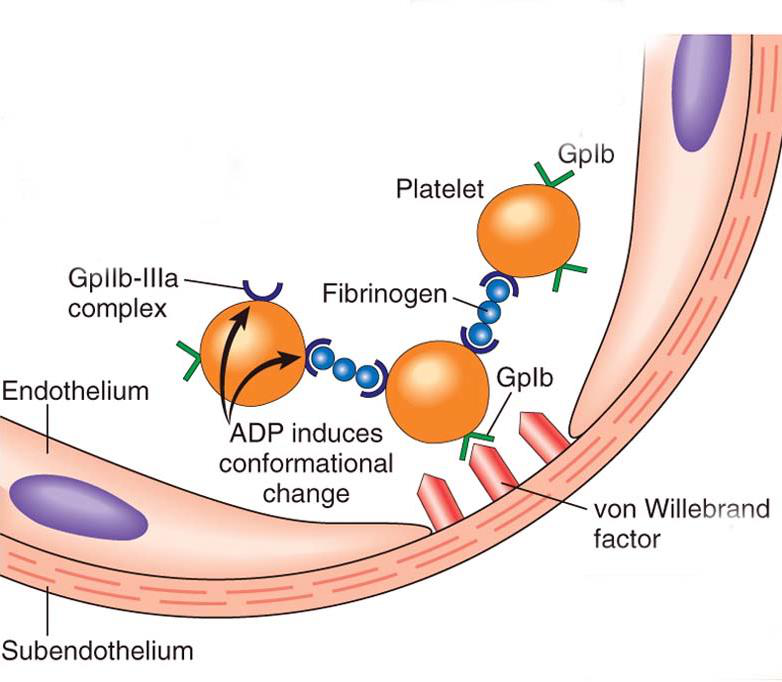
What triggers activation of the platelet membrane glycoprotein complex GPIIb/IIIa and what is its primary function?
- Trigger: Platelet activation causes membrane activation of the glycoprotein complex IIb/IIIa
- Primary function: Acts to cause platelet aggregation
-
Which major ligands does the platelet receptor GPIIb/IIIa bind?
- Ligands: von Willebrand factor (VWF) and fibrinogen
-
What is the consequence of GPIIb/IIIa deficiency for platelet function at a vessel injury site?
- Platelet plug fails to accumulate at the site of vessel injury when GPIIb/IIIa is absent.
-
Which clinical disorder is caused by deficiency of the GPIIb/IIIa receptor?
- Glanzmann's thrombasthenia
-
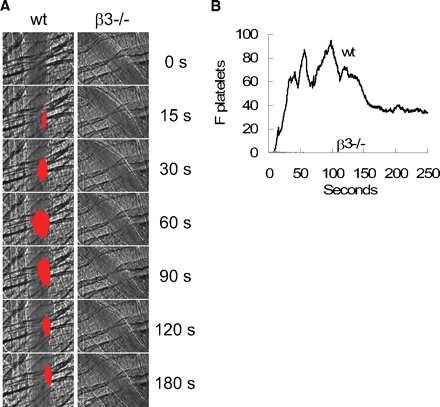
How does platelet aggregation compare between wild-type and beta3-deficient (3-/-) subjects in the provided experiment?
- Beta3-deficient (3-/-) subjects show reduced platelet aggregation compared with wild-type (wt).
Answer image:
-
-
What is the primary mechanism of action of abciximab on platelets?
- Blocks GPIIb/IIIa, thereby inhibiting platelet aggregation
-
What is the main clinical use of abciximab described in the text?
- Prevents formation of blood clots during procedures to open blocked arteries
Platelets — quick overview
- Definition: Small, anucleate cell fragments from megakaryocytes that patrol the vasculature and respond to injury.
- Size: \(2\)–\(4\,\mu m\).
- Lifespan: \(\sim 10\ \text{days}\).
- Normal count: \(150\)–\(400\times 10^9\ \text{L}^{-1}\).
- Function: maintain vascular integrity, form primary haemostatic plug after injury.
Ultrastructure & key components
- Major compartments: phospholipid membrane, open canalicular system (OCS), mitochondria, dense granules, alpha granules.
- Surface receptors (important): GPIb-IX-V complex, GPVI, GPIIb/IIIa.
- Dense granules: contain Ca2+, ADP/ATP, serotonin — promote activation and recruitment.
- Alpha granules: contain VWF, fibrinogen, factor V, platelet factor 4 — supply clotting and adhesive proteins.
Image — platelet ultrastructure

How platelets find and stick to injured vessel (adhesion)
- First step: exposed subendothelial matrix (e.g., collagen) at injury site captures circulating proteins and platelets.
- Key mediator: Von Willebrand factor (VWF) — a multimeric plasma protein that must tether/unravel to expose platelet-binding sites.
- When VWF unravels it exposes binding sites for GPIba (part of the GPIb-IX-V complex) and for collagen.
Image — VWF unwinding

GPIb-IX-V complex (platelet receptor)
- Composed of subunits GPIba, GPIb, GPIX, GPV and linked to the cytoskeleton.
- Function: binds unfolded/tethered VWF under high shear, initiating platelet tethering and slowing of platelets near the lesion.
Image — GPIb-IX-V schematic

VWF–GPIba interaction — why it matters
- Under high shear (arteries), direct platelet adhesion to collagen is inefficient; VWF acting through GPIba is essential.
- If VWF tethering or GPIba binding is impaired, platelet adhesion at sites of high shear fails and bleeding occurs.
Important clinical defects in adhesion
- Von Willebrand disease (VWD): most common bleeding disorder; caused by quantitative (low VWF) or qualitative (impaired binding to collagen/platelets) defects in VWF.
- Bernard–Soulier syndrome: rare genetic defect in GPIb\/a (GPIb-IX-V) that prevents normal VWF interaction and causes bleeding tendency.
Platelet activation — overview
- Activation converts a quiescent platelet into a haemostatic cell capable of adhesion, secretion, and aggregation.
- Four main changes on activation:
- Shape change (discoid → spherical with pseudopodia).
- Activation of integrins (notably GPIIb\/IIIa).
- Granule secretion (dense and alpha granules).
- Phospholipid "flip-flop" exposing anionic surface.
Image — platelet shape change (SEM)

1) Shape change
- Occurs within seconds after adhesion; actin and microtubule reorganisation produces spherical shape and filopodia to increase surface contact and stability.
2) Granule release
- Dense granules: release small-molecule agonists (ADP, Ca2+, serotonin) that amplify activation and recruit platelets.
- Alpha granules: release adhesive and clotting proteins (VWF, fibrinogen, factor V, PF4) to support aggregation and coagulation.
Open canalicular system (OCS)
- Membrane invaginations forming tunnels linking interior granules to the surface; acts as a conduit for rapid secretion and membrane expansion during activation.
Image — OCS (platelet surface invaginations)

3) Phospholipid "flip-flop"
- Activation externalises negatively charged phospholipids (e.g., phosphatidylserine) previously on the inner leaflet.
- This anionic surface is required for assembly/binding of several coagulation complexes and vitamin K–dependent factors on the platelet surface.
Image — lipid bilayer and flip-flop

4) GPIIb\/IIIa activation and platelet aggregation
- GPIIb\/IIIa (integrin αIIbβ3) undergoes a conformational change on activation, allowing it to bind fibrinogen and VWF and cross-link adjacent platelets, forming an aggregate.
- Without functional GPIIb\/IIIa, platelets cannot form a stable plug (see Glanzmann thrombasthenia).
Image — GPIIb\/IIIa interacting with fibrinogen/VWF

Clinical correlates related to aggregation
- Glanzmann thrombasthenia: genetic deficiency of GPIIb\/IIIa → defective aggregation and mucocutaneous bleeding.
- GPIIb\/IIIa inhibitors (e.g., Abciximab): monoclonal antibodies that block the receptor to prevent platelet aggregation during coronary interventions.
Image — aspirin (common platelet inhibitor)

Pharmacologic inhibition of platelet activation
- Aspirin: irreversibly inhibits COX-1 in platelets, reducing thromboxane A2 synthesis and impairing activation/aggregation.
- GPIIb\/IIIa antagonists (Abciximab): block final common pathway of platelet aggregation.
Key takeaways (high-yield)
- Platelet adhesion under high shear relies on VWF tethering and the GPIb-IX-V receptor.
- Activation causes shape change, granule release, phospholipid externalisation, and integrin activation (GPIIb\/IIIa) — together produce aggregation and support coagulation.
- Major disorders: VWD (VWF defects), Bernard–Soulier (GPIb defect), Glanzmann thrombasthenia (GPIIb\/IIIa defect).
- Antiplatelet drugs target different stages: aspirin (activation signaling) and GPIIb\/IIIa inhibitors (aggregation).
Quick self-test questions
- What receptor mediates VWF-dependent adhesion under high shear?
- Which granule type releases ADP and serotonin?
- Name two clinical syndromes caused by defects in GPIb or GPIIb\/IIIa.