Sign up to unlock more features
- Save this deck to your account
- Study flashcards with spaced repetition
- Export to Anki (.apkg) or PDF
- Process documents up to 100 pages
- Images extracted from PDFs and documents
- Better text extraction from your PDFs and documents
- Better flashcards with our more advanced AI model
Flashcards in this deck (43)
-
In 1609, what observation described the first case of Hemolytic Disease of the Newborn (HDN)?
- A set of twins: one was hydropic and stillborn
- The other twin was jaundiced and died of kernicterus
history hdn -
Before 1939, what limitation in blood typing was noted despite correct ABO matching?
Concern was limited to ABO only, yet there were still reports of mortality and morbidity including Hemolytic Transfusion Reactions (HTR) and Hemolytic Disease of the Fetus and Newborn (HDN)
history abo -
What key findings in the 1939 Levine and Stetson case suggested a non-ABO antigen?
- An obstetrical patient had an HTR after transfusion from her husband despite same ABO
- Mother's serum antibody reacted at 37°C and 20°C with the father's RBC
- Her serum reacted with 80 of 104 ABO-compatible donors
history levine -
What did Landsteiner and Wiener report in 1940 about antibodies produced in animals with Rhesus macaque RBCs?
- Animals produced an antibody that reacted on 85% of human RBCs
- The antigen causing this antibody was named 'Rh' after the Rhesus monkey
 discovery rh
discovery rh -
What Rh pattern did Levine find in over 90% of erythroblastosis fetalis cases in 1941?
The mother was Rh-negative and the father was Rh-positive
levine erythroblastosis -
According to Levine, what caused erythroblastosis fetalis in the 1941 findings?
Maternal antibody caused erythroblastosis fetalis after the mother was immunized by a fetus carrying an antigen inherited from the father
hdn immunology -
What later distinction was made between human anti-Rh and animal anti-Rh?
Human anti-Rh and animal anti-Rh were proven not the same; the animal anti-Rh was renamed 'anti-LW'
rh lw -
How did Fisher name Rh antigens in 1941?
He named C and c based on reactivity of two antibodies and used the next letters D and E to define antigens recognized by two additional antibodies
fisherrace nomenclature -
What was Fisher's 1943 proposal about the genetic basis of Rh antigens?
That antigens of the system were produced by three closely linked sets of alleles, each gene producing an antigen on the RBC surface
genetics fisherrace -
According to Fisher-Race, what set of Rh genes does a person inherit?
One D or d, one C or c, and one E or e (one set inherited from each parent)
genetics inheritance -
What are the reported gene frequencies of common Rh antigens in Caucasians?
- D = 85%
- d = 15%
- C = 70%
- E = 30%
- c = 80%
- e = 98%
genetics frequencies -
Why was the Rh phenotype reported in the order 'DCE' in 1946?
Because Fisher thought the C/c locus lies between the D/d and E/e loci
fisherrace nomenclature -
In Fisher-Race notation, what does the 'd' symbol represent?
The 'd' does not represent an antigen but simply the absence of the D antigen
fisherrace notation -
What does placing parentheses around (D), (C), and (e) indicate in Fisher-Race terminology?
Parentheses indicate a weakened antigen expression
notation fisherrace -
Which Rh terminology was followed for written communication historically?
The Fisher-Race terminology was followed for written communication
fisherrace communication -
rh genetics weiner
-
According to Dr. Weiner, what does the Rh gene produce?
An agglutinogen containing a series of blood factors
rh agglutinogen genetics -
How many factors did Dr. Weiner state the Rh gene produces within an agglutinogen?
At least 3 factors
rh factors genetics -
How may Rh be considered in relation to the haplotype?
Rh may be considered the phenotypic expression of the haplotype
 rh haplotype phenotype
rh haplotype phenotype -
nomenclature
-
nomenclature
-
In the Rh shorthand, what do '1' (single prime) and '2' (double prime) indicate?
- 1 (single prime) = presence of C
- 2 (double prime) = presence of E
nomenclature -
nomenclature
-
rosenfield nomenclature
-
According to Rosenfield, how is an antigen's absence indicated?
- A 'minus sign' preceding the number designates absence
rosenfield nomenclature -
What else did Rosenfield's alphanumeric terminology state about its genetic basis?
- It has no genetic basis and does not involve a theory of Rh inheritance; it simply demonstrates presence or absence of antigen
rosenfield nomenclature -
How does the ISBT six-digit number encode antigen information?
- First 3 digits represent the system; last 3 represent antigenic specificity
isbt nomenclature -
isbt
-
What were the two early theories of Rh genetic control mentioned?
- Wiener: single gene produces a single product with separately recognizable factors
- Fisher-Race: Rh locus contains 3 distinct genes that control production of their respective antigens
genetics theories -
Which gene codes for the RhD protein and what notable feature flanks it?
- RHD gene codes for RhD protein; RHD is flanked by Rhesus boxes
rhd genetics -
rhce genetics
-
What is stated about most Rh-negative white people regarding RHCE?
- Most Rh-negative white people have only the RHCE gene
population genetics -
On which chromosome is RHAG found and how similar is it to RH genes?
- RHAG is found on chromosome 6 and is 47% identical to the RH genes
rhag genetics -
rhag structure
-
rhag protein
-
List the key functional facts about RHAG from the text.
- Similar in structure to Rh proteins but has a glycoprotein
- Forms a complex with Rh proteins for successful expression (coexpressor)
- By itself it does not express Rh antigen
- If mutated, Rh proteins will be missing or altered
rhag function -
Where are RH and RHAG mRNAs found according to the text?
- RH and RHAG mRNAs are found only in erythroid lineage cells
expression -
Describe the order of appearance of RHAG and Rh proteins during erythropoiesis.
- RHAG appears early in CD34+ progenitors; Rh proteins appear later (RhCE then RhD)
erythropoiesis -
What evolutionary origin is proposed for RHAG and Rh genes?
- RHAG and Rh genes are believed to have arisen from gene duplication 250-350 million years ago
evolution -
How are Rh antigens defined and how important is the D Rh system?
- Rh antigens are cell surface antigens on RBCs; the 'D' Rh system is one of the most important blood group systems, second only to ABO
definition importance -
genetics diagram
-
genetics diagram
-
Which diagram can help visualize Rh proteins in the erythrocyte membrane?
- Diagram of protein structure embedded in erythrocyte surface
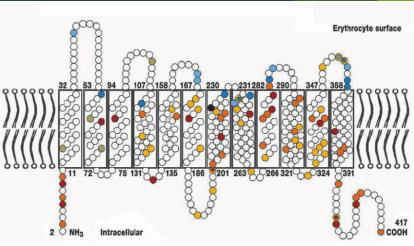 diagram structure
diagram structure
RH blood group — overview
- The Rh blood group is a major RBC antigen system second only to ABO and is central to transfusion medicine and hemolytic disease of the fetus and newborn (HDN).
History (key events)
- 1609: First description of HDN in twins (one hydropic stillborn, one jaundiced died of kernicterus).
- 1930s: Focus was mainly on ABO; unexplained HTRs and HDN occurred despite ABO compatibility.
- 1939 (Levine & Stetson): Described HTR in an obstetrical patient; maternal antibody reacted with paternal RBCs and many ABO-compatible donors.
- 1940 (Landsteiner & Wiener): Animal antisera made against Rhesus macaque RBCs reacted with ~85% human RBCs — named "Rh" after rhesus monkeys (animal anti-Rh later renamed anti-LW).
- 1941 (Levine): Found most erythroblastosis fetalis cases had Rh‑negative mothers and Rh‑positive fathers; maternal antibodies from fetal immunization caused the disease.

Key clinical concepts
- Hemolytic transfusion reaction (HTR): immune-mediated RBC destruction after transfusion when incompatible antigens are present.
- Hemolytic disease of the fetus and newborn (HDN): maternal alloantibody (IgG) against fetal RBC antigens causing fetal/neonatal hemolysis; classic example involves anti‑D.
- Maternal immunization: mother lacking an antigen (e.g., D) can form antibody after exposure to fetal RBCs that carry that antigen.
Terminology systems for Rh
1) Fisher–Race (DCE terminology)
- Proposes three closely linked loci producing antigens: D/d, C/c, E/e; alleles are codominant.
- Antigen letters: D, C, c, E, e. The lowercase d denotes absence of D (not a real antigen).
- Typical phenotype determined by combination of expressed antigens.
- Reported approximate gene frequencies (Caucasians):
- D = 85% • d = 15%
- C = 70% • c = 80%
- E = 30% • e = 98%
- Fisher used the order D–C–E to describe phenotype.
2) Wiener (Rh–hr terminology)
- Suggested a single gene produces a multi-factor agglutinogen (multiple factors within one product).
- Introduced symbols like R, r, R1, R2, R0 to denote haplotypes (historical notation; reflects phenotypic haplotypes).
3) Rosenfield (alphanumeric)
- Assigns numbers to antigens for serologic/computer readability: D=1, C=2, E=3, c=4, e=5.
- Presence indicated by number; absence by a minus sign before the number.
4) ISBT (international numeric)
- Standardized nomenclature giving each antigen a 6‑digit code; Rh system assigned 004 as the system number.
Molecular biology & genetics
Genes and loci
- The Rh antigens are coded mainly by two genes on chromosome 1: RHD and RHCE; these genes are highly homologous (~97% identity).
- RHD encodes the RhD protein (D antigen).
- RHCE encodes the C/c and E/e antigen variants (combinations like Ce, cE, ce, CE).
- Many Rh‑negative Caucasians lack a functional RHD and retain only RHCE at the two loci.
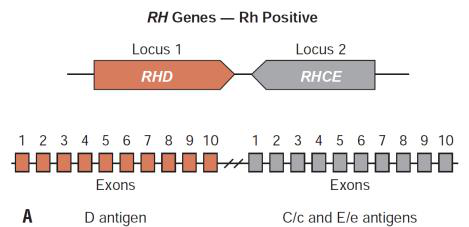
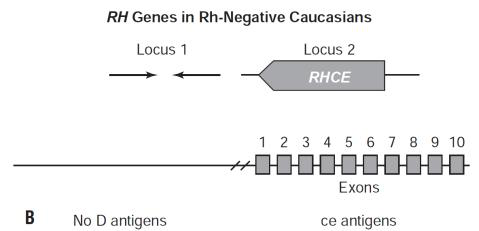
RHAG (Rh-associated glycoprotein)
- RHAG on chromosome 6 encodes Rh‑associated glycoprotein (Rh50), a coexpressor required for normal Rh protein expression.
- RHAG alone does not carry Rh antigens but forms complexes with Rh proteins; mutations can disrupt Rh surface expression.
- RH and RHAG mRNAs are restricted to erythroid cells; RHAG appears early in progenitors followed by RHCE then RHD during erythropoiesis.
Origin & expression
- RH and RHAG likely arose by gene duplication 250–350 million years ago.
- RHD is flanked by Rhesus boxes which play a role in gene deletion events that produce Rh negativity in some populations.
Antigen variants: Weak D and Partial D
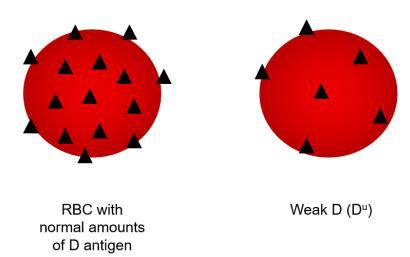
- Weak D (Du): reduced quantitative expression of D antigen on RBCs; can be from mutations that lower surface D density.
- Partial D: qualitative changes where parts (epitopes) of the D antigen are missing; patients can form anti‑D to epitopes they lack.
- Laboratory note: Weak or partial D may give variable serologic reactions; differentiation often requires molecular testing or specialized panels.
- Clinical implication: Partial D individuals may be at risk of alloimmunization if exposed to full D epitopes.
Practical/clinical implications
- Transfusion: correctly identifying D status is essential; weak/partial D complicate typing and may require extra testing.
- Pregnancy: an Rh‑negative mother can become sensitized by an Rh‑positive fetus and form IgG anti‑D that causes HDN in subsequent pregnancies.
- Serology vs genetics: serologic methods detect antigen expression, while molecular tests identify underlying RHD/RHCE variants.
Study/practice tips
- Memorize Fisher–Race antigens (D, C/c, E/e) and that d = absence of D.
- Remember RHD and RHCE are separate but homologous genes; RHAG is required for expression.
- Distinguish weak D (low density) from partial D (missing epitopes) — both affect clinical decisions.
References / further reading (from source)
- Historical work by Levine, Stetson, Landsteiner, Wiener, Fisher; ISBT nomenclature and molecular studies of RHAG and RHD/RHCE.